Tejaswi Kanala MD
1.2K posts


Tejaswi Kanala MD
@TSKanala
RadOnc | Fellow @MDAndersonNews | @RadOncTMC, OsmaniaMed alum | @CanGenetics_TMC | Organ preservation & Radiobiology | opinions my own |

Disruptive Analysis of Total Neoadjuvant Therapy in Locally Advanced Rectal Cancer: Clinical and Therapeutic Distinctions Between Low- and Mid-Rectal Cancers. Read the full article. ascopubs.org/doi/abs/10.120… #gicsm


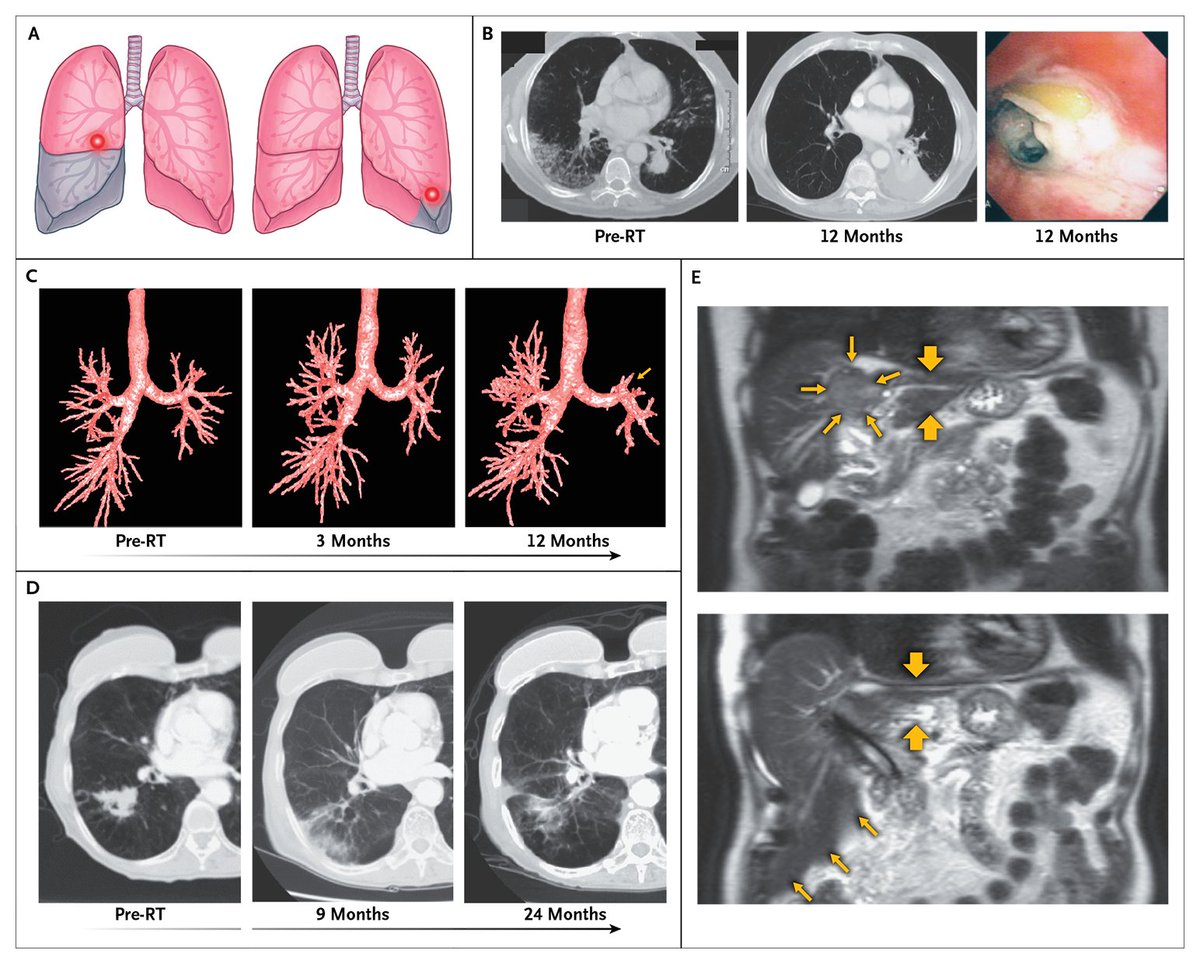

@DavidSherMD I also think this whole discussion points out a misdirection of intellectual resources and radiation oncology. I think this infatuation with technology that is relatively minor has diverted the intellectual efforts of the field.



85 years of care, compassion, and commitment. Since 1941, @TataMemorial has remained dedicated to accessible cancer care, advancing research, and training the next generation of oncology professionals. Honouring the legacy. Renewing the commitment. #85YearsOfCare #FoundationDay




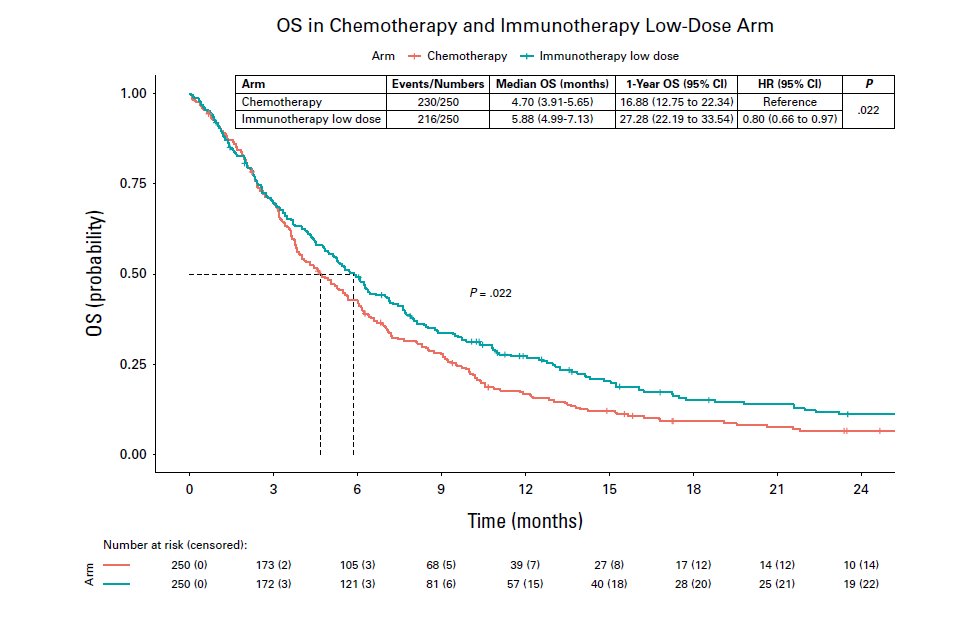
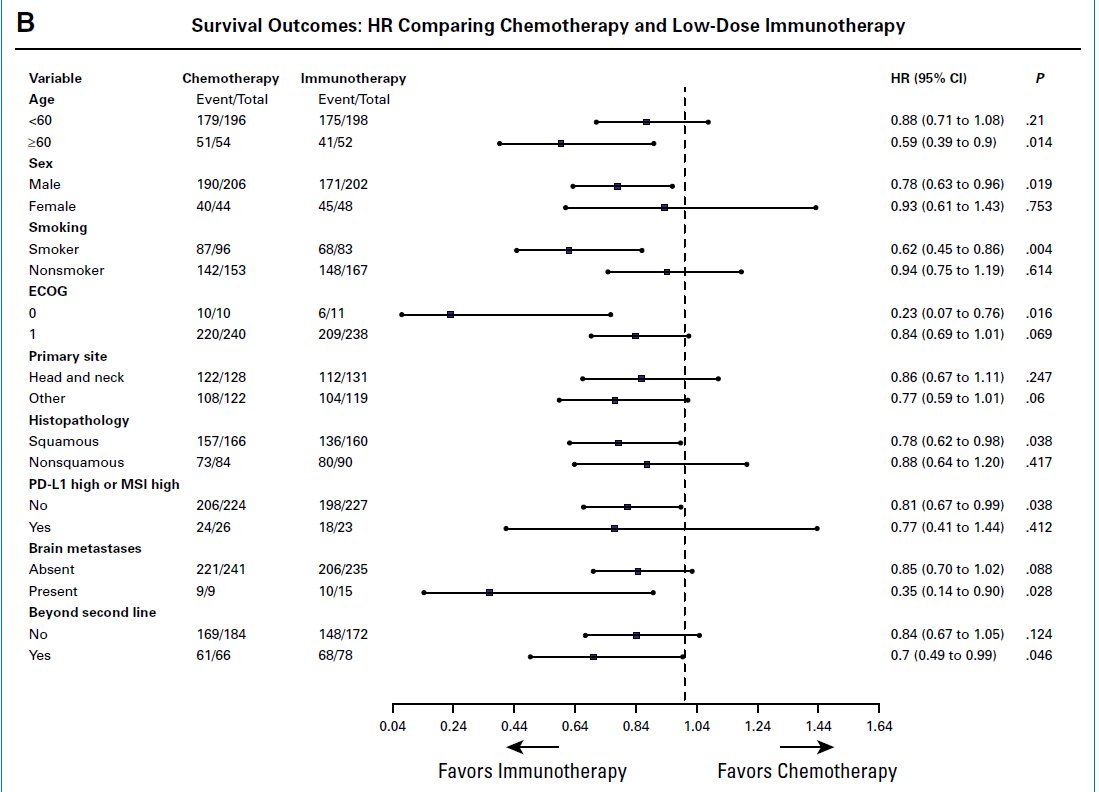


An absolutely damning indictment of the costs of care (in the fiscal meaning of the word): just as many patients fear financial toxicity as death! #GI26













