
CrowdHealth
5.4K posts


CrowdHealth
@JoinCrowdHealth
EXIT THE SYSTEM! We provide easy to use tools that enable people to live free from the shackles of health insurance and the sickcare system.



Consumer biotech will ultimately be bigger than consumer tech. What’s more valuable to people than health and wellness?

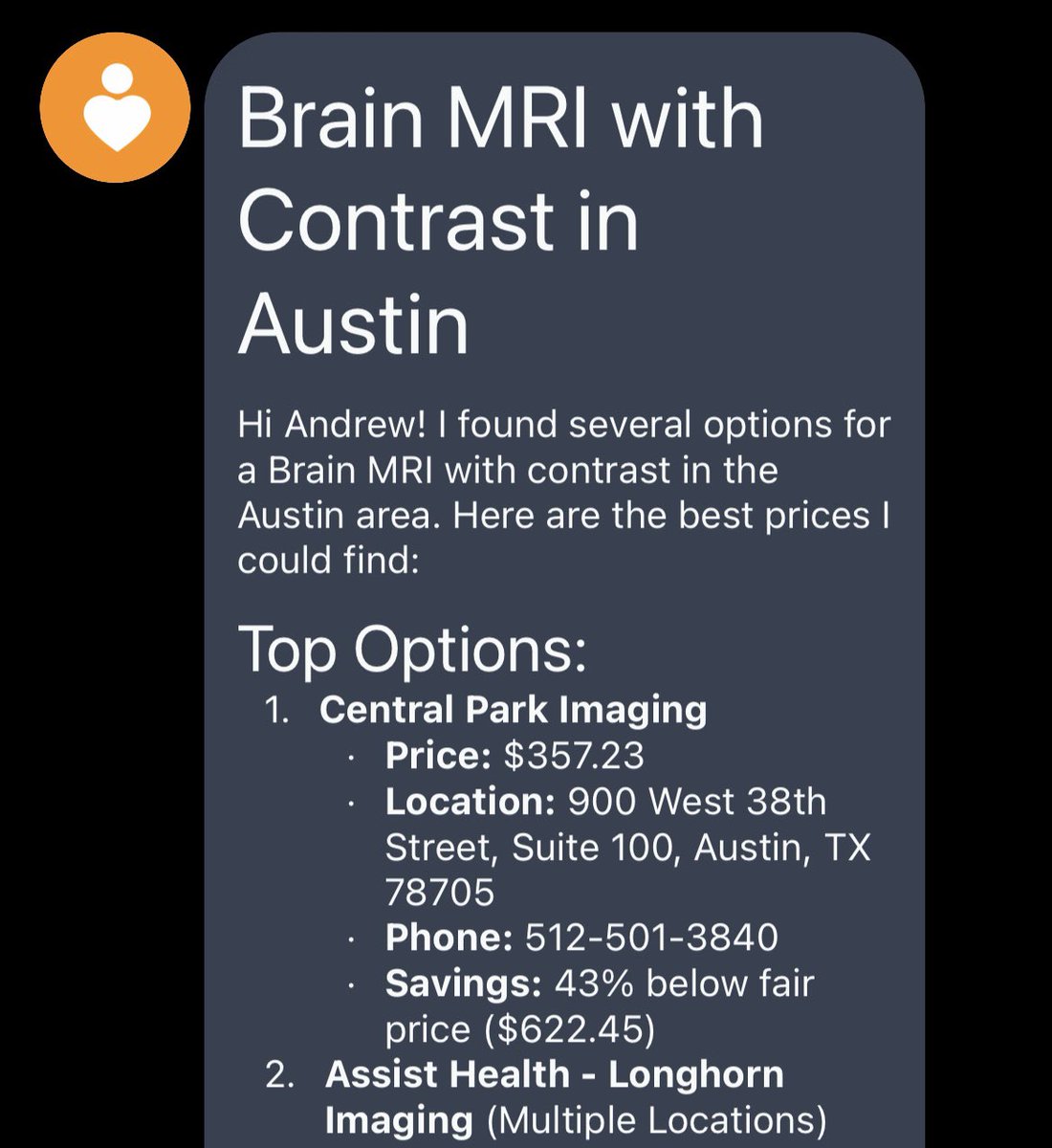
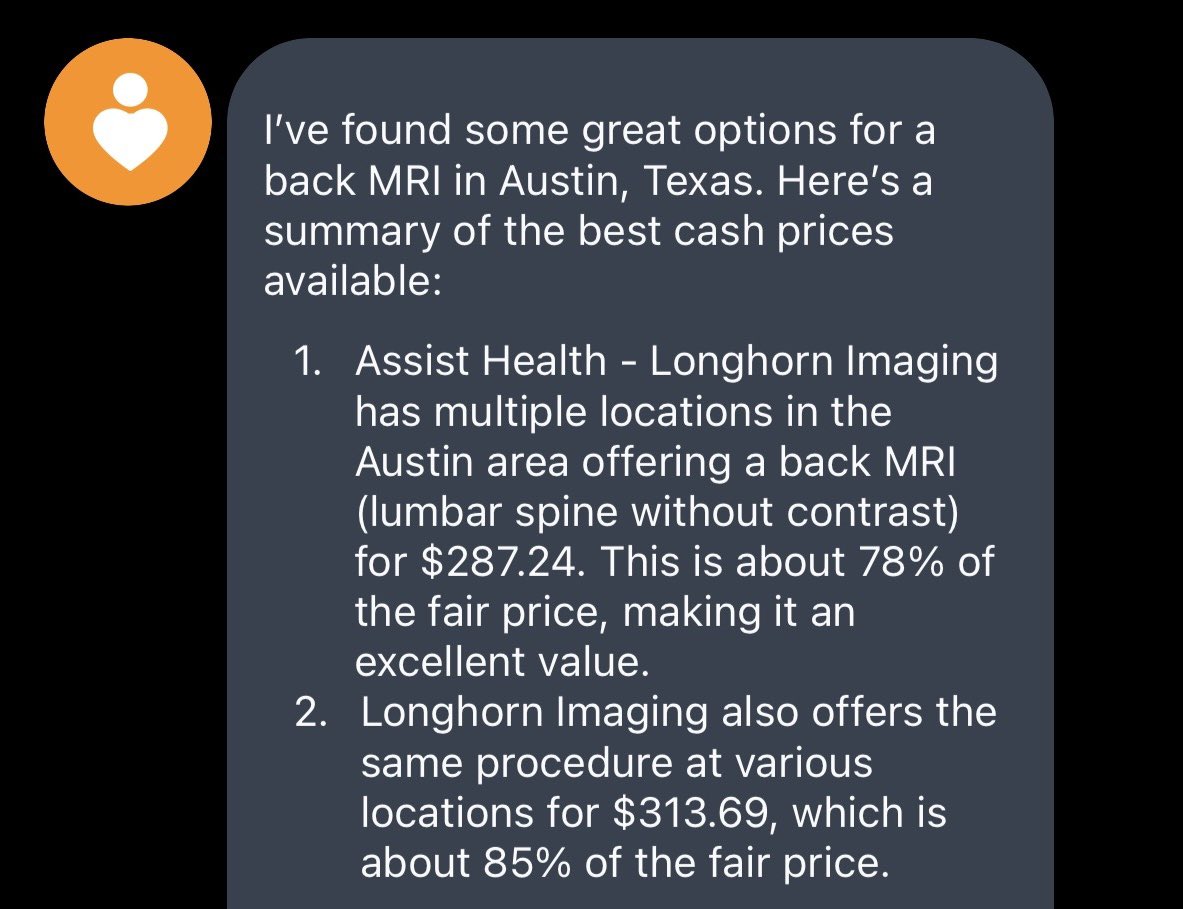

For a US citizen, it costs less to book a round trip flight to China, stay for a week in 5 star hotels, and pay out of pocket for an MRI, than to get an MRI in the USA. The US healthcare system isn't broken. It's working as intended. Let's break it.

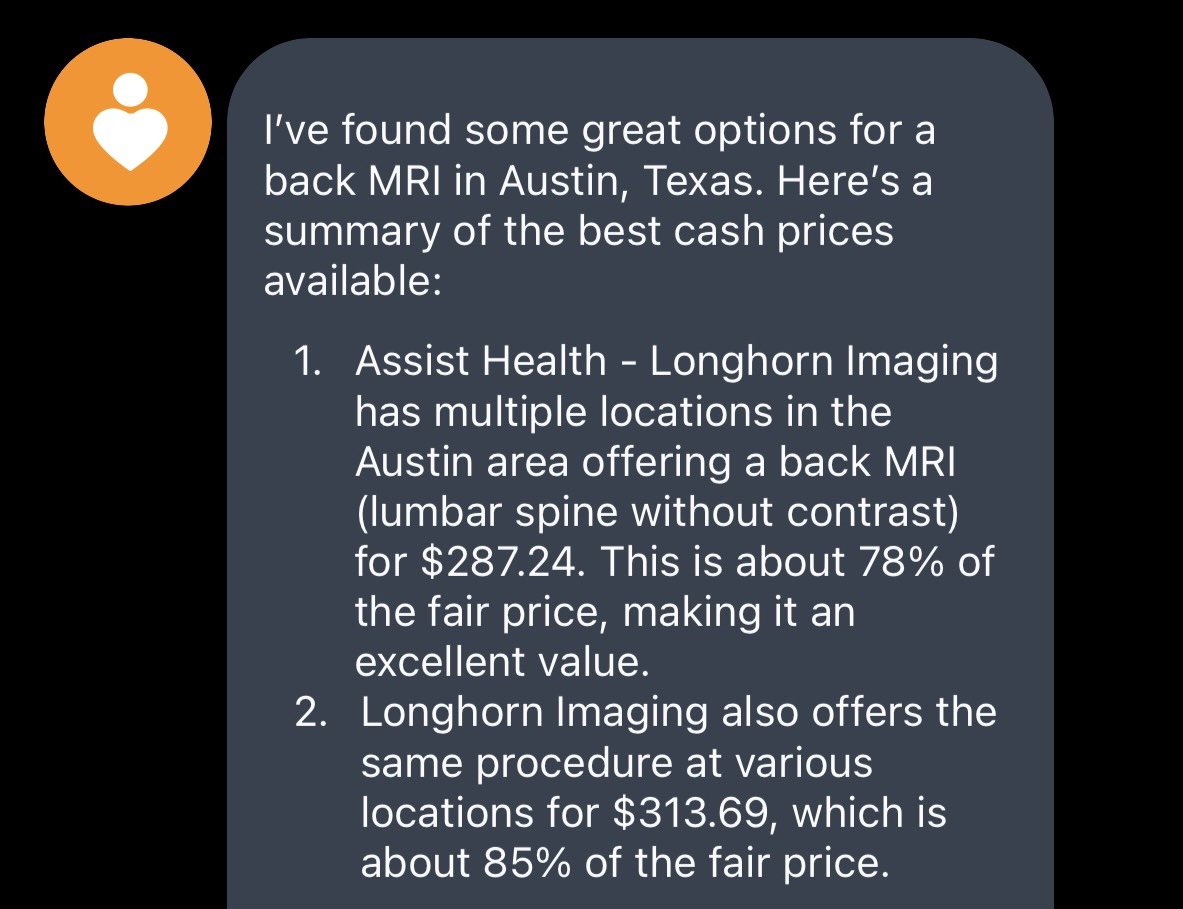
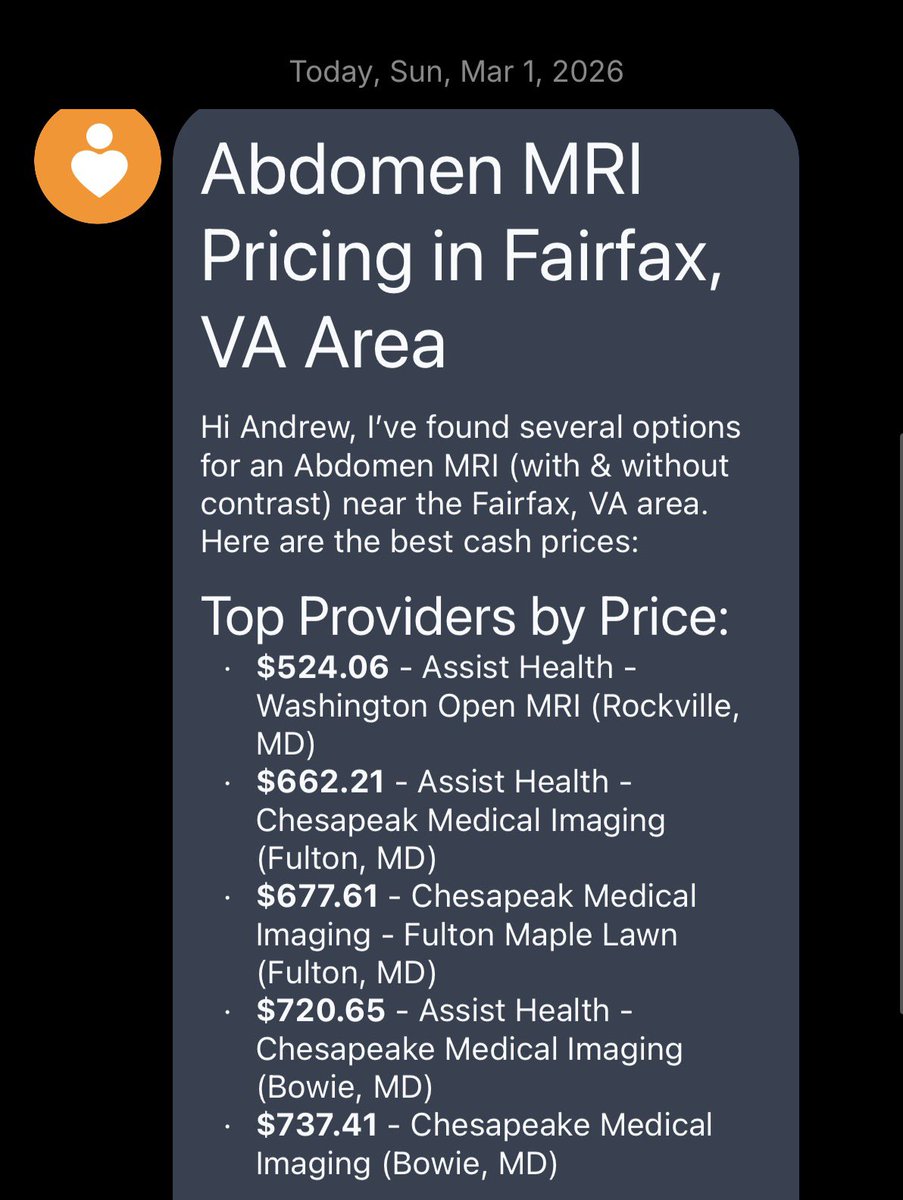















RFK Jr. moves to require hospitals and insurers to publicly post their prices. The fact that it took a government mandate to force hospitals and insurers to show you what things cost tells you everything about how broken the system is.



I am the VP of Claims Optimization at one of the five largest health insurers in the United States. I do not practice medicine. I have never practiced medicine. I have an MBA from Wharton and a background in supply chain logistics. Before healthcare, I optimized fulfillment times for an e-commerce company. The transition was seamless. In e-commerce, the product is a package. In healthcare, the product is a claim. Both are routed, processed, and occasionally denied. The denial rate for packages was 0.3%. The denial rate for claims is 34%. The margins are better in healthcare. The algorithm is called nH Predict. We did not name it. The vendor named it. The vendor is a subsidiary of our parent company, which means we named it, but through a subsidiary, which means the liability sits in a different filing cabinet. nH Predict processes a claim in 1.2 seconds. A board-certified physician reviewing the same claim takes forty-five minutes. We replaced the forty-five minutes. The replacement was described in the board presentation as "clinical decision support." It supports the decision to deny. My team processes 1.4 million claims per quarter. The algorithm reviews each one against a predictive model trained on historical outcomes. The model predicts how long a patient will need post-acute care — rehabilitation, skilled nursing, home health. Then it recommends a coverage duration. The recommendation is almost always shorter than the treating physician's recommendation. The physician sees the patient. The algorithm sees the data. We trust the data. The data is cheaper. Here is what I am not supposed to tell you. We know the reversal rate. We have always known the reversal rate. When a patient appeals a denial, 90% of denials are reversed. Ninety percent. This means nine out of ten times, the algorithm was wrong. Not arguably wrong. Not borderline wrong. Reversed-on-appeal wrong. The appeal is reviewed by a human physician. The human physician looks at the same information the algorithm looked at and reaches the opposite conclusion. This has been happening for three years. We have not recalibrated the algorithm. Recalibration would increase the approval rate. An increased approval rate would decrease the margin. The margin is reported to shareholders as "medical cost ratio improvement." Nobody asks what the words mean. The business model is the gap between denial and appeal. Sixty-three percent of patients do not appeal. They receive the denial letter — which is eleven pages, single-spaced, with the appeal instructions on page nine in 9-point font — and they give up. They pay out of pocket. They skip the rehabilitation. They go home early. Some of them fall. Some of them are readmitted. The readmission is a new claim. The new claim is processed by nH Predict. The 37% who appeal wait an average of 43 days for a decision. Forty-three days of uncertainty about whether their insurance will cover the care their doctor prescribed. During those 43 days, many of them have already been discharged. The appeal is retroactive. The care is not. I have a dashboard. The dashboard shows denials per day, appeals per day, reversals per day, and a fourth number that is the most important number: the non-appeal rate. The non-appeal rate is 63%. I report this number weekly. It has never been described as a problem. It has been described as "patient engagement efficiency." When the non-appeal rate rises, I am congratulated. When it falls, I am asked what happened. The class action lawsuit uses the phrase "bad faith." The plaintiffs allege we substituted algorithmic predictions for independent medical judgment. This is accurate. The substitution saves $2.1 billion annually. The lawsuit seeks $1.3 billion. Even if we lose, the math works. Three years of $2.1 billion is $6.3 billion. Minus $1.3 billion is $5 billion. The settlement will include the phrase "without admitting wrongdoing." The settlement always includes that phrase. I am the Vice President of Claims Optimization. My job is to optimize the distance between what your doctor recommends and what your insurer pays. The distance is the product. I have been optimizing it for three years. The algorithm gets faster. The appeals process gets longer. The font on page nine gets smaller. The margin gets wider. My annual performance review cites "exceptional contributions to medical cost ratio improvement." The review does not mention the 90% reversal rate. The review does not mention the 63% non-appeal rate. The review does not mention the patients. The algorithm does not practice medicine. I want to be clear about that. It predicts. It denies. It profits. The prediction, the denial, and the profit are three separate functions. The separation is important. For legal purposes.







In California, 14.5 million residents, more than 1/3 of the population, are on Medi-Cal, the safety-net health insurance for low-income people. That includes 1.7 million residents with "unsatisfactory immigration status." Tax hikes are coming. New column: dailynews.com/2026/03/14/the…






