Mark Piehl
83 posts


@markpiehl
Intensivist @WakeMed Medical Director @WakeMed Children's Mobile Critical Care Founder & Chief Medical Officer @410Medical











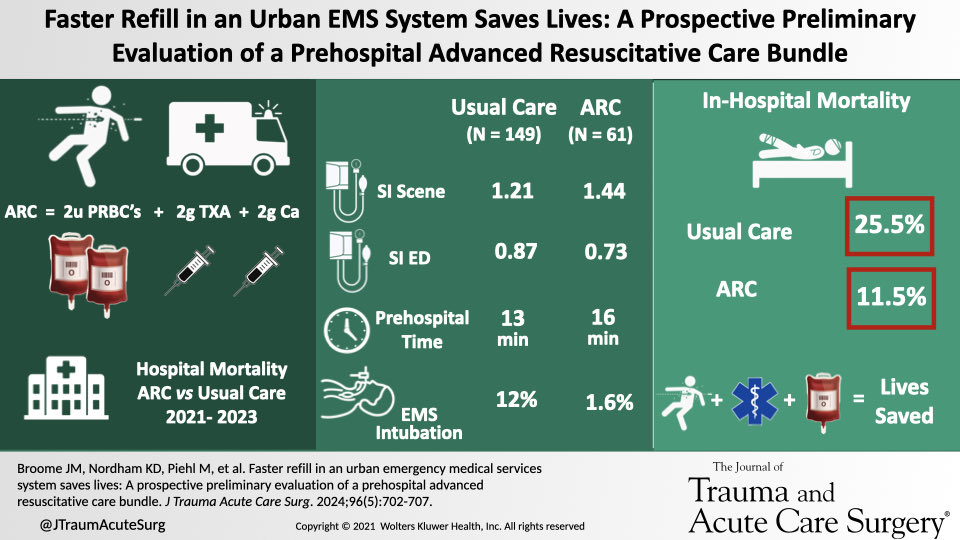
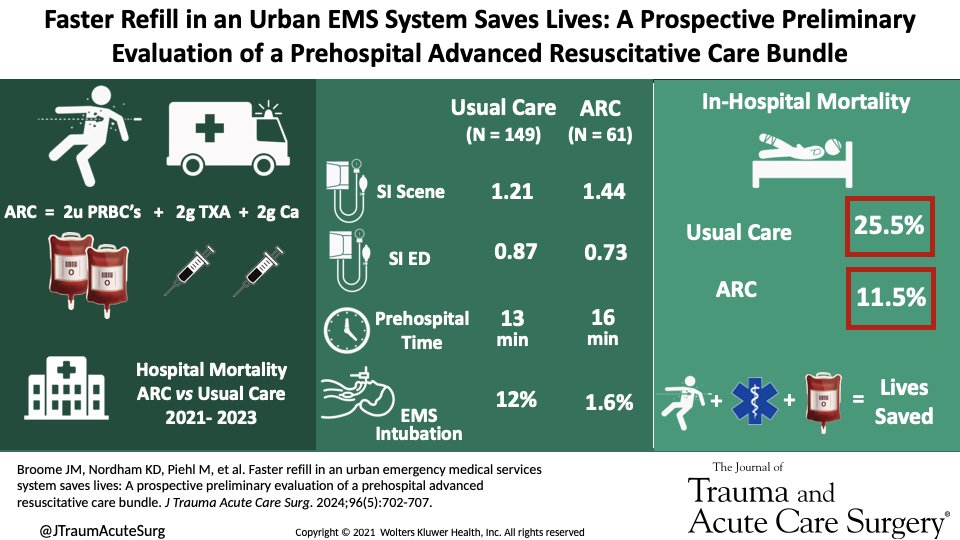
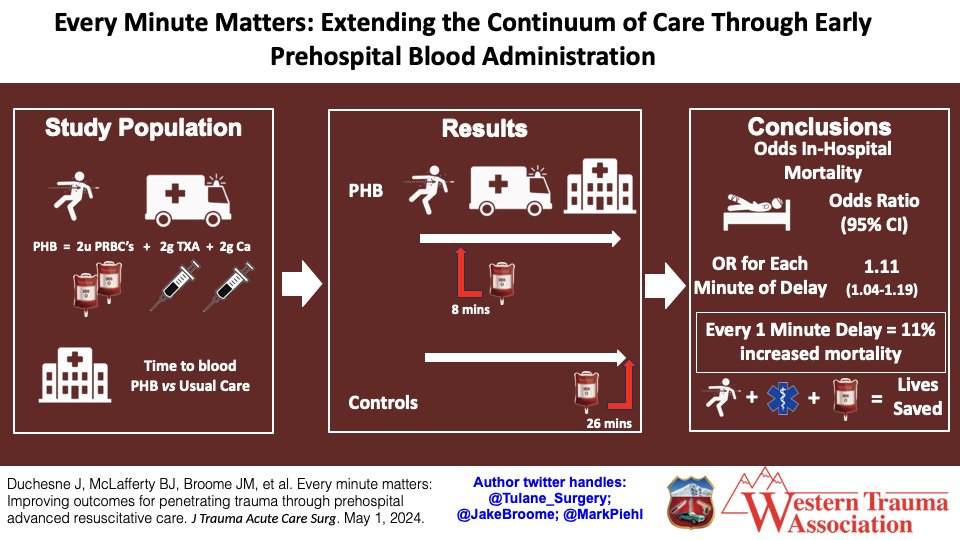
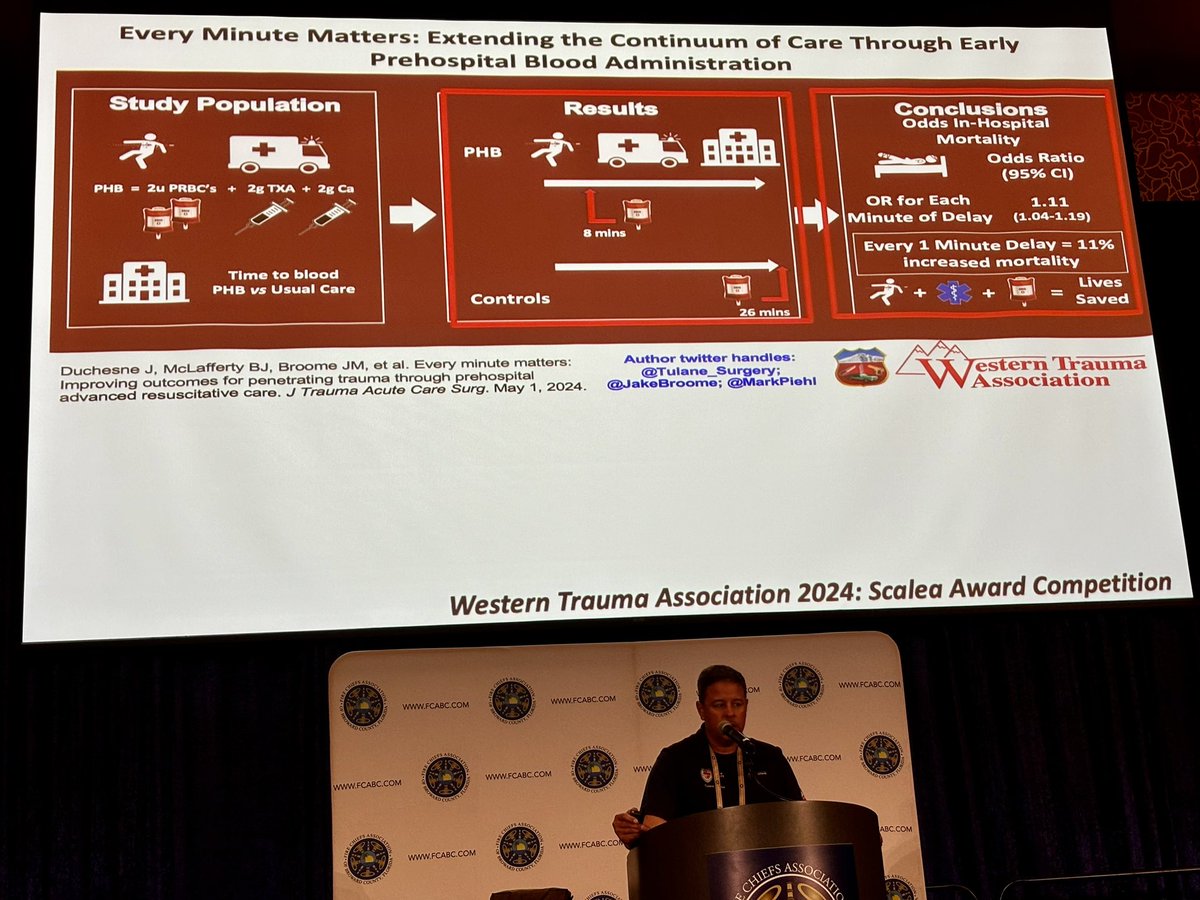
🚨 New Episode Alert! 🚨 Can prehospital blood save lives? 💉 Dr. Jeff Jarvis dives into the "ARC Bundle" (blood, TXA, calcium) and its impact on trauma care with an 81% mortality reduction. 🎧 Listen now at flightbridgeed.com/emslhp-podcast or on your favorite platform!

Does your EMS system carry #WholeBlood? In only 7 months @dcfireems has administered blood to 162 patients BEFORE they arrived at the hospital. Of the patients who weren't already in cardiac arrest, 93% survived. Full report here: tr.ee/kAMgpF1a0j Join us on Friday to hear from Lt. Holly O'Byrne. @EMSPhysician | @QinfloWarrior | @LifeFlow__ | @markpiehl | @RandiSchaefer8 | @PhilSpinellaMD | @noemsf | @PBCFR | @CH1PBCFR | @Chief5PBCFR | @CoralSpringsFD | @DavieFireRescue | @SATXFire | @my1blood | @AABB | @JonKrohmer

Everyone in EMS should take the time to read this… Then go do it. Every day you wait, people in your community are missing out on a lifesaving resource.






Meta-analysis from Dr. Schoenfeld found no significant one-month mortality benefit to civilian-setting prehospital transfusion. This should give pause to EMS systems considering transfusion programs #EMS #Transfusion @BIDMCEM #AEM #EM