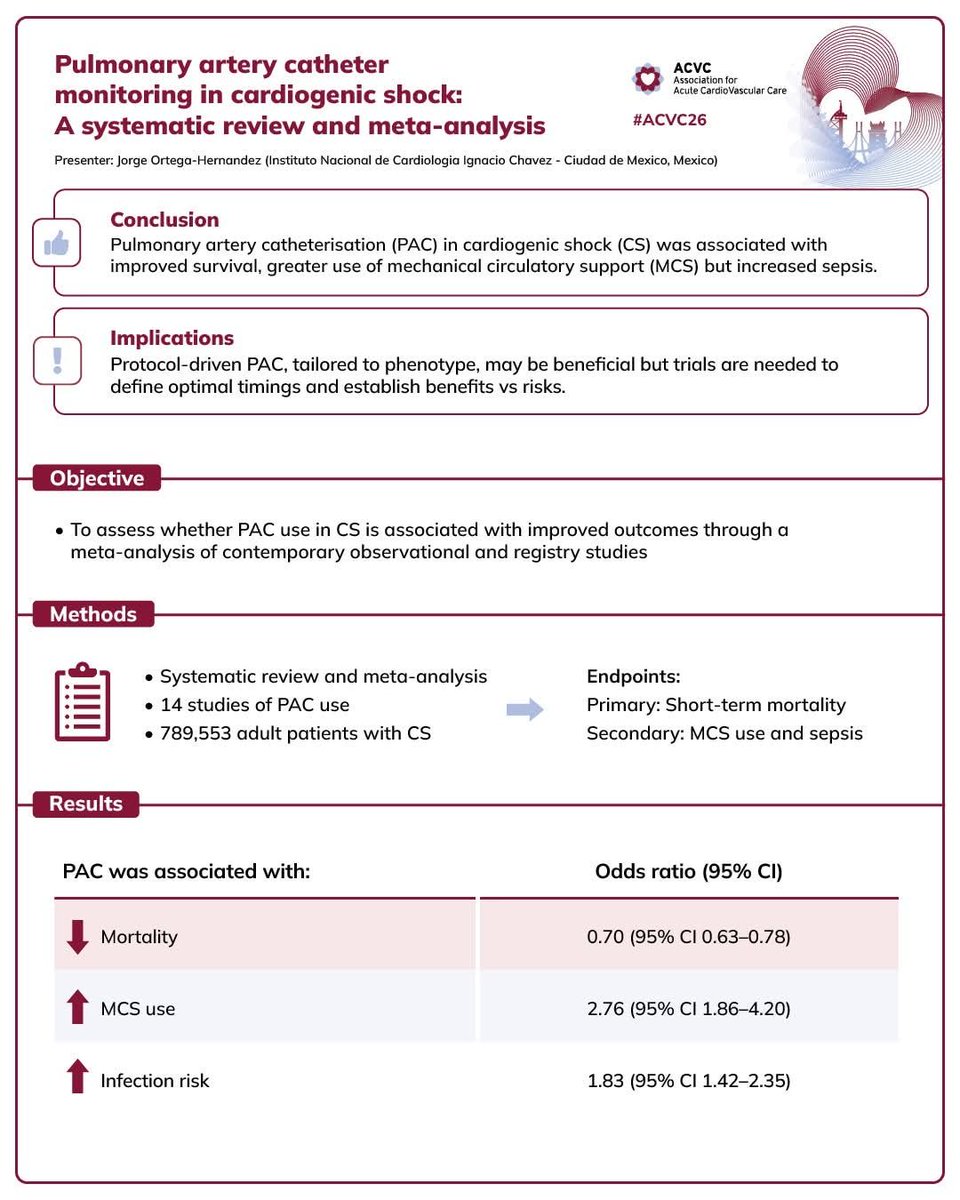
#ACVC 2026: Mixed shock: the reality behind cardiogenic shock An outstanding session by Dr. David Morrow. Morrow highlighting a critical and often under-recognized concept: 👉 Pure cardiogenic shock is rare. Mixed shock is common. 🔍 Key messages: SVR is not always elevated in cardiogenic shock → Wide variability, often with vasoplegia (SIRS component) Mixed shock = low CO + inappropriately low SVR → A combination of cardiac failure + vasodilatory physiology 📊 Epidemiology (SHARC data): .Cardiogenic shock (isolated): ~65% .Mixed shock: ~17% .Mortality highest in mixed shock (~48%) 🧠 Common phenotypes: -Cardiogenic shock → secondary vasoplegia -Cardiac arrest → stunned myocardium + vasodilation -Sepsis + cardiac dysfunction -Toxic cardiomyopathy (e.g., Ca-blockers, BBs) -Post-cardiotomy vasoplegia ⚙️ Pathophysiology: Inflammation (SIRS) plays a central role Microcirculatory dysfunction + iNOS activation Loss of vascular tone despite vasopressors ⚠️ Clinical implication: 👉 Hemodynamics must be interpreted dynamically, not assumed 👉 SVR ≠ always high → avoid “one-size-fits-all” approach 🛠️ Management principles: Phenotype-guided therapy Combine: Vasopressors (norepinephrine first-line) Inotropes when needed Careful fluid strategy Consider: .Methylene blue / hydroxocobalamin in refractory vasoplegia .CIRCI (steroids) in selected patients 📌 Take-home message: Cardiogenic shock is not purely cardiac. Recognizing the vasoplegic component is key to survival. #ACVC26 #CardiogenicShock #MixedShock #CriticalCare #Hemodynamics #ShockManagement