@inthehm01 @CoffeeBlackMD There has never been a trial of albumin vs no-albumin in HRS. I suspect in the ICU where we can give vasopressors easily it makes absolutely no difference
English
Ivor Popovich
964 posts

@InternSupp
NZ Intensivist. Physiology geek. Book author, “A Dim Prognosis.” https://t.co/PP58ZrN5SI


Taking acetaminophen, also known by the brand name Tylenol, during pregnancy had no effect on children developing autism, according to a study of over 1.5 million children in Denmark published this week. abcnews.link/W8uhOQ1






What is the most reasonable immediate next step?




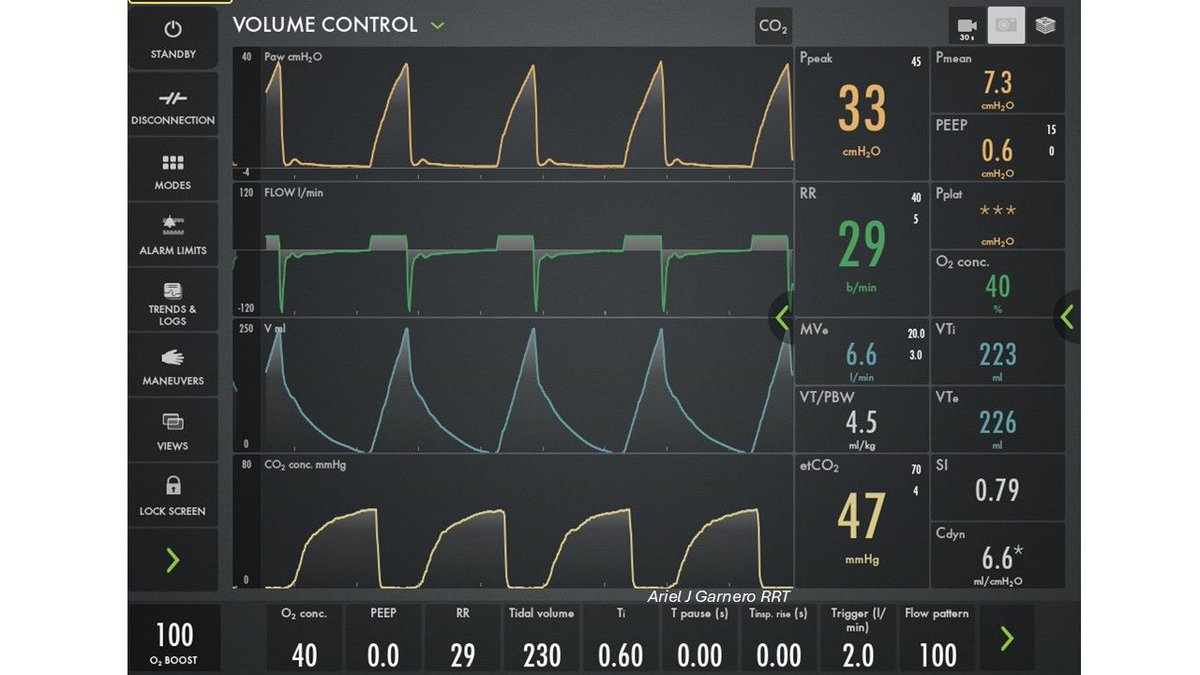










The success rate of “idk try an inotrope” has to be sub 5%* *even for intermediate physiologic outcomes