Prof Peter Collignon
36.6K posts

Prof Peter Collignon
@CollignonPeter
Infectious Diseases Physician and Microbiologist. Professor Medical School. Australian National University. Views are my own.


The new weight loss drugs are roughly as effective for blood pressure-lowering as anti-hypertensives:







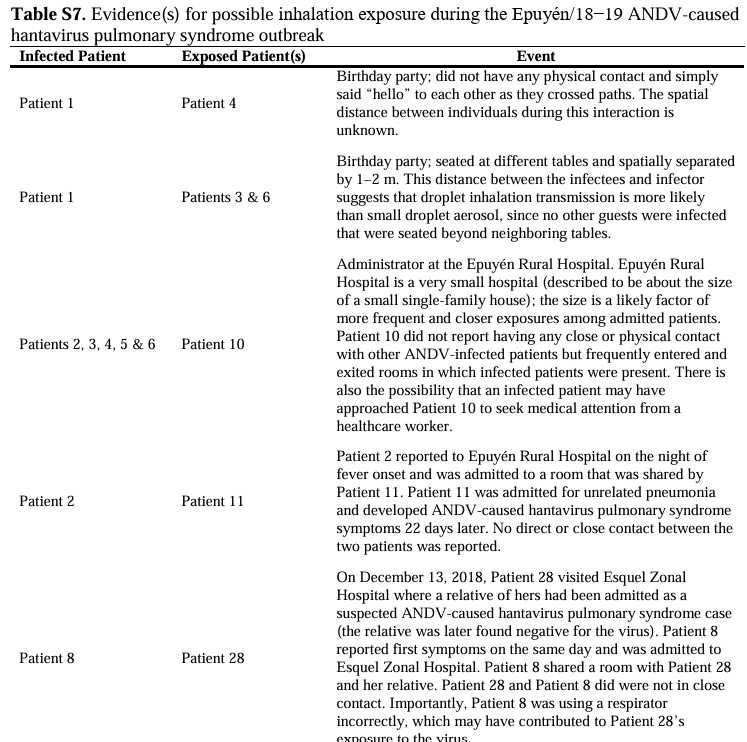
Harvard Professor @j_g_allen says past hantavirus outbreaks did not require “prolonged close contact”: “One person passed it to another person at a birthday party simply by passing by and saying hello.”


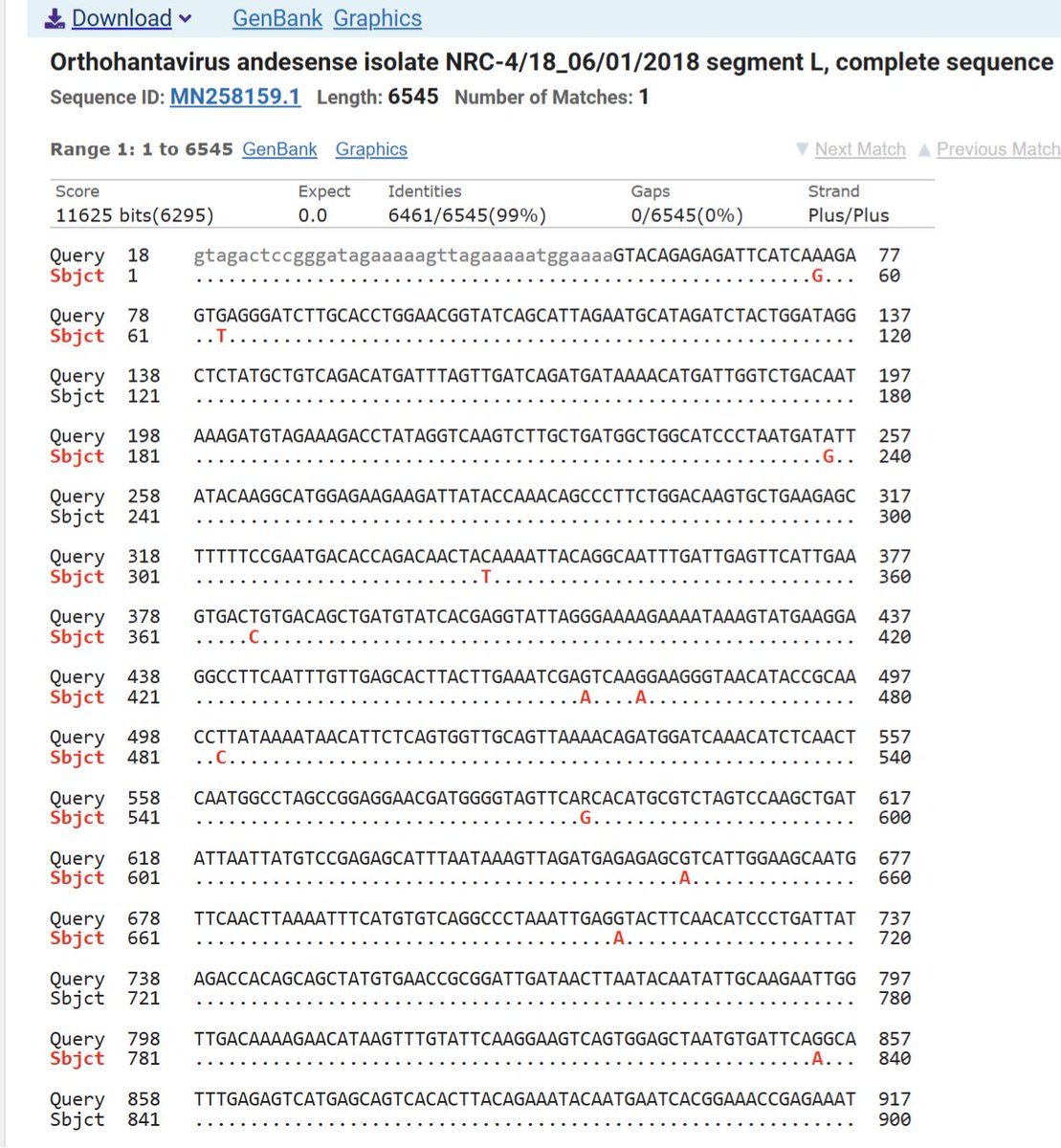
BREAKING: First sequencing of the Hantavirus from the outbreak. -99% identical to a June 2018 case from a patient in Argentina -10.4 SNV/year mutation rate - The Andes genome is about 12 kb across three RNA segments. At 10⁻⁴ to 10⁻³ substitutions/site/year, that translates very roughly to 1-12 SNV per year -Completely in line with a natural spillover in Argentina from the rodent host in 2018 and now in 2026 Source: virological.org/t/complete-seq…

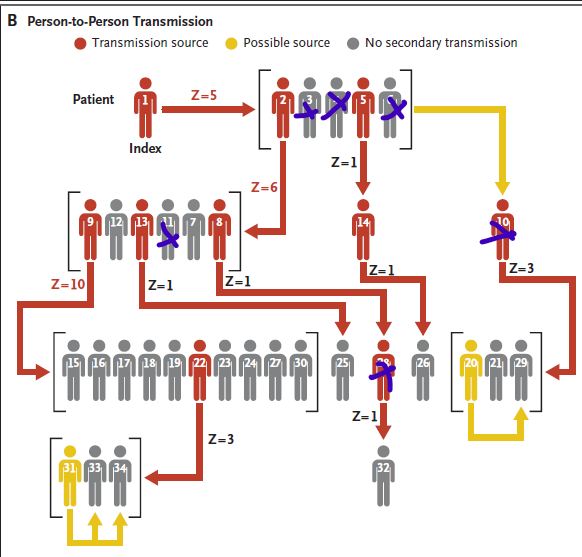
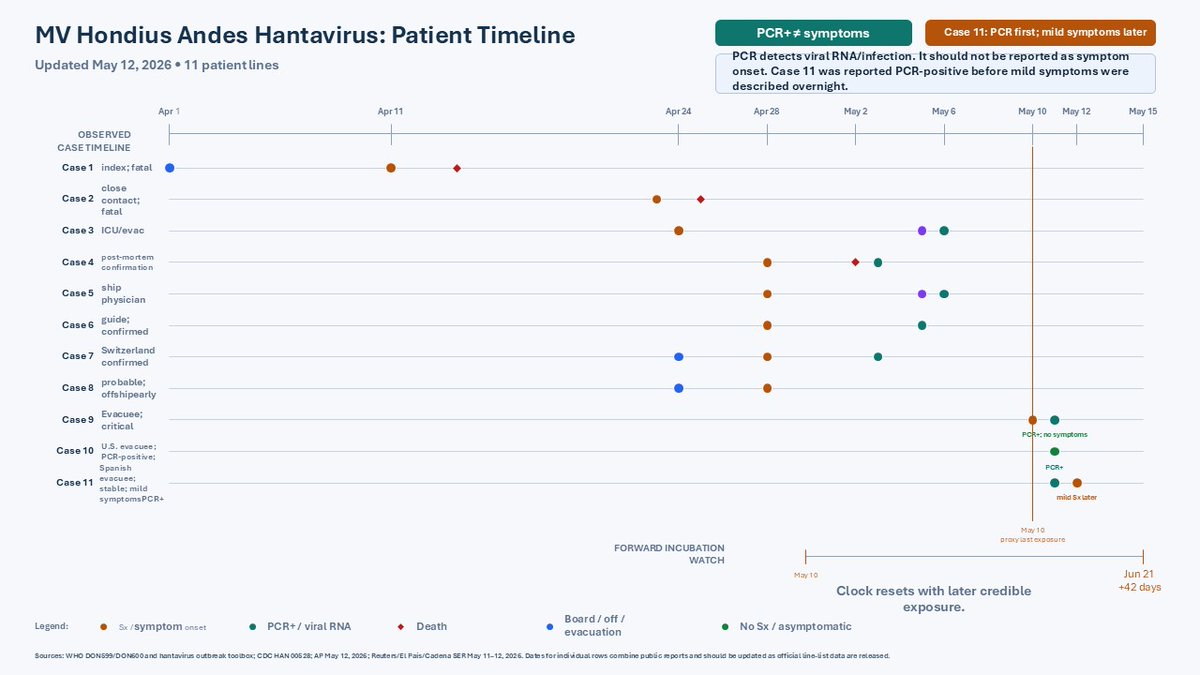
That hentavirus superspreading paper is really interesting, full of detail. It enables evidence for many narratives and those who favour one or another can certainly get evidence. Airborne transmission - yep possible. But so is close contact families sharing homes, let's look:


Great article from Carl Heneghan and Tom Jefferson, voices of reason during COVID. "Hantavirus is a rare disease. In the United States, which diligently tracks such cases, there have been 890 laboratory-confirmed instances since 1993. In the UK, the situation is even less clear: from 2012 to early 2025, only 11 domestically acquired symptomatic cases have been recorded. Surprisingly, nine of these cases were not linked to cruise ships or exotic travel, but rather to a more mundane source - exposure to “pet fancy rats” or rodents bred as reptile feed. This is not a pathogen ready to spread through the Home Counties. However, the rarity is not the issue; visibility is." Link in comments.





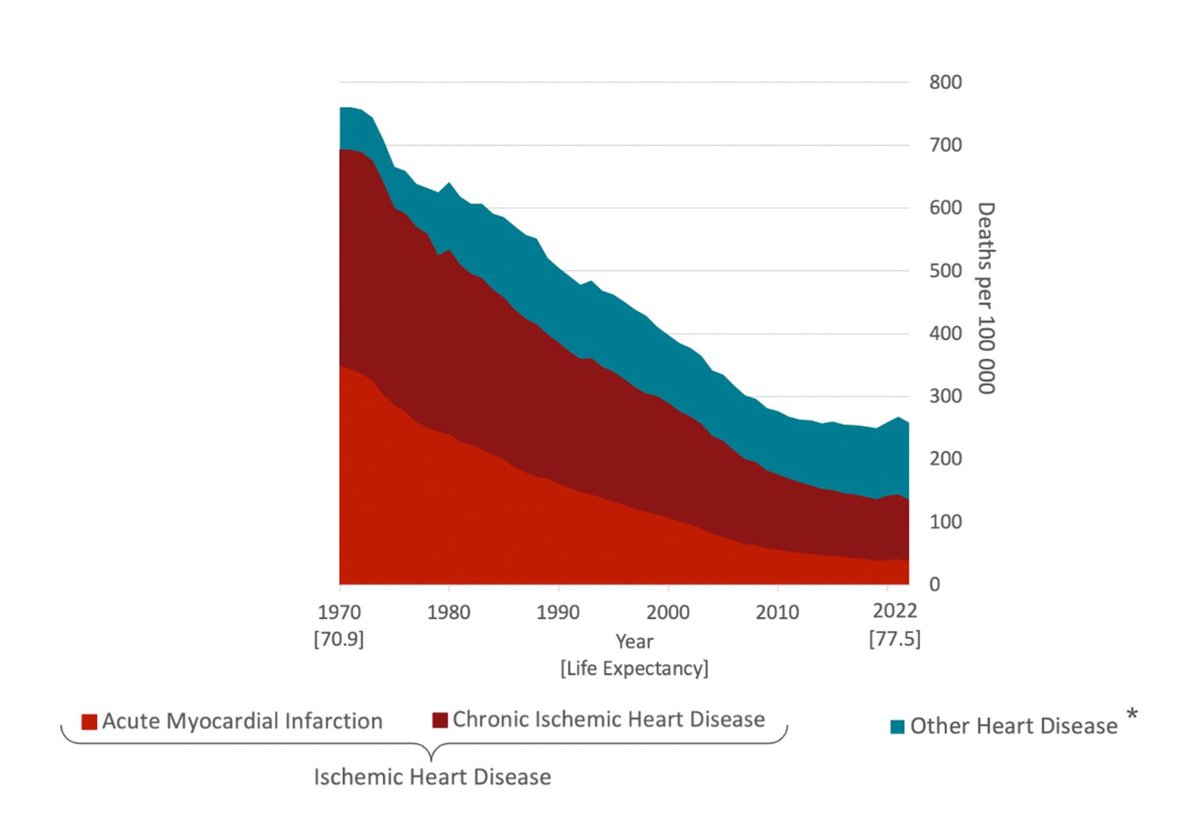
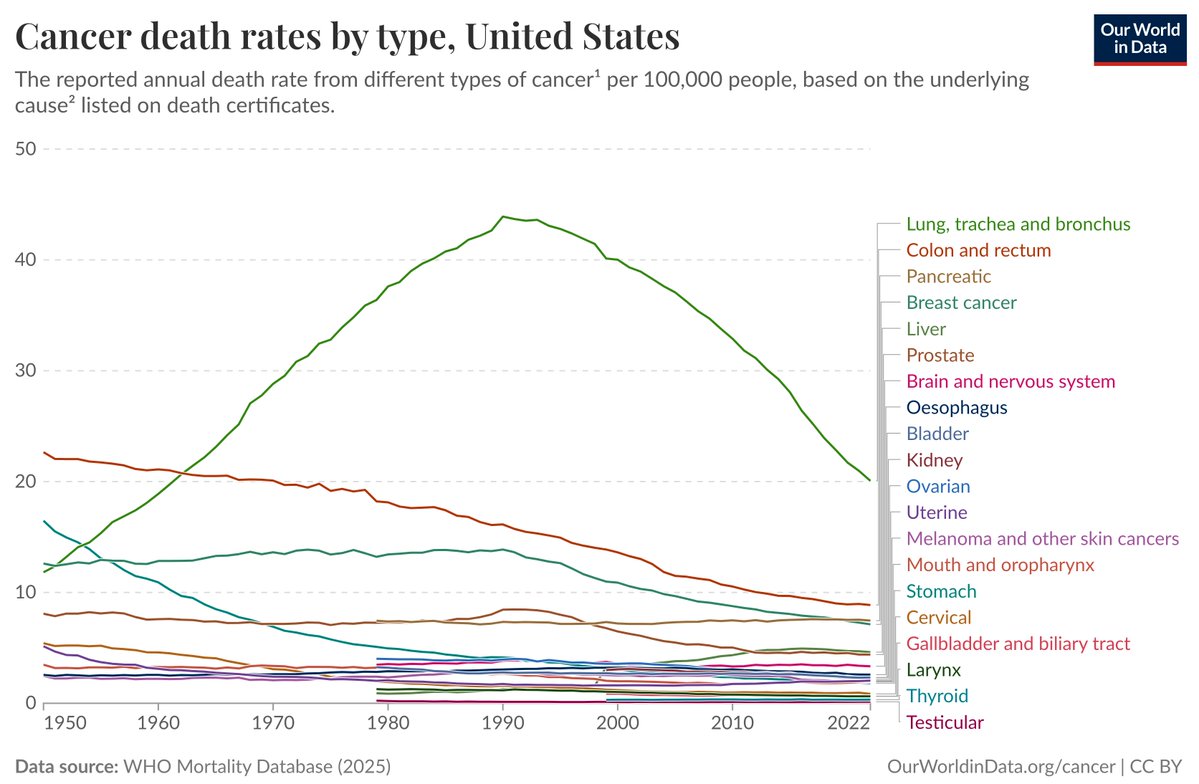
Heart disease has been the number one killer of people in this country for 30 plus years. And it shows no signs of change.