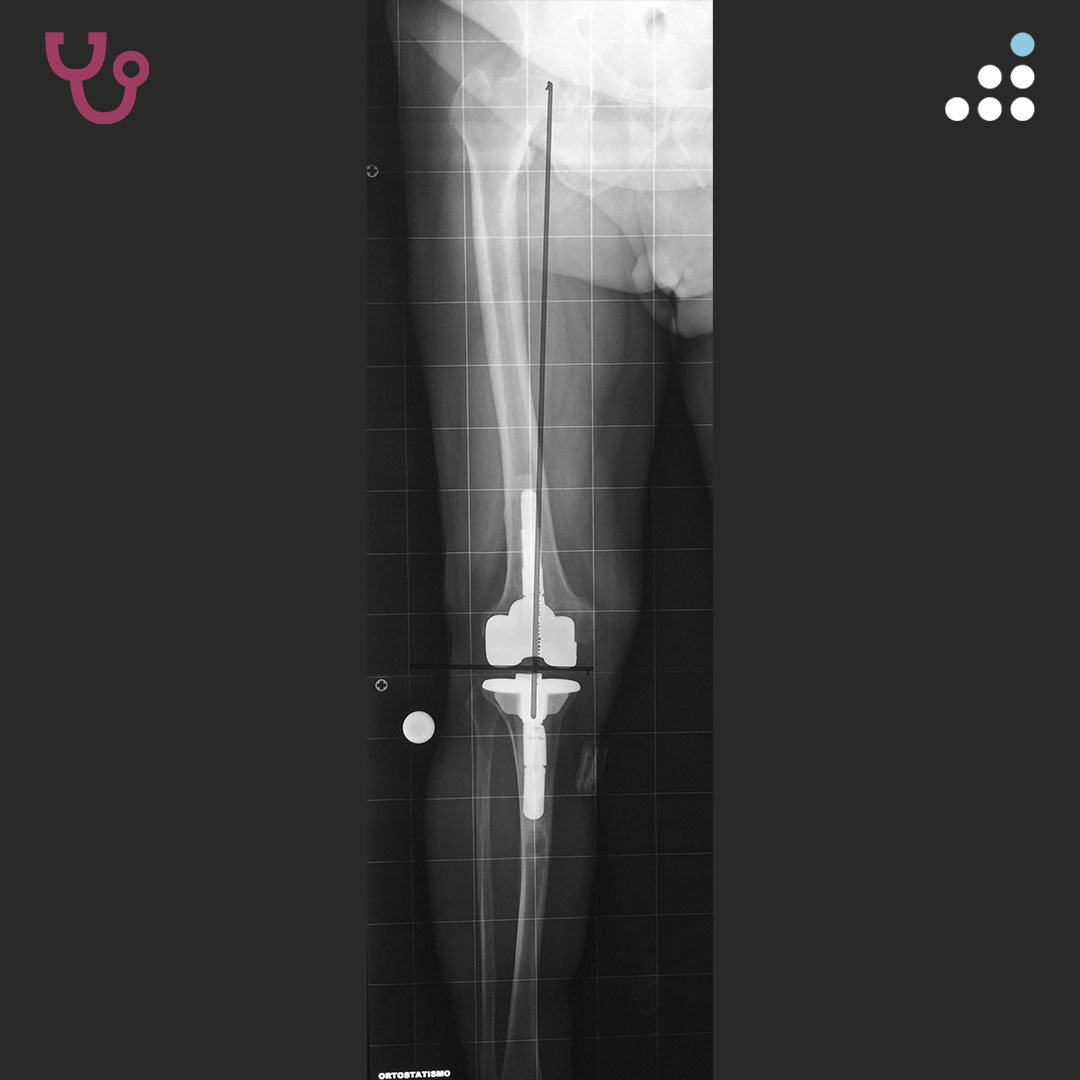
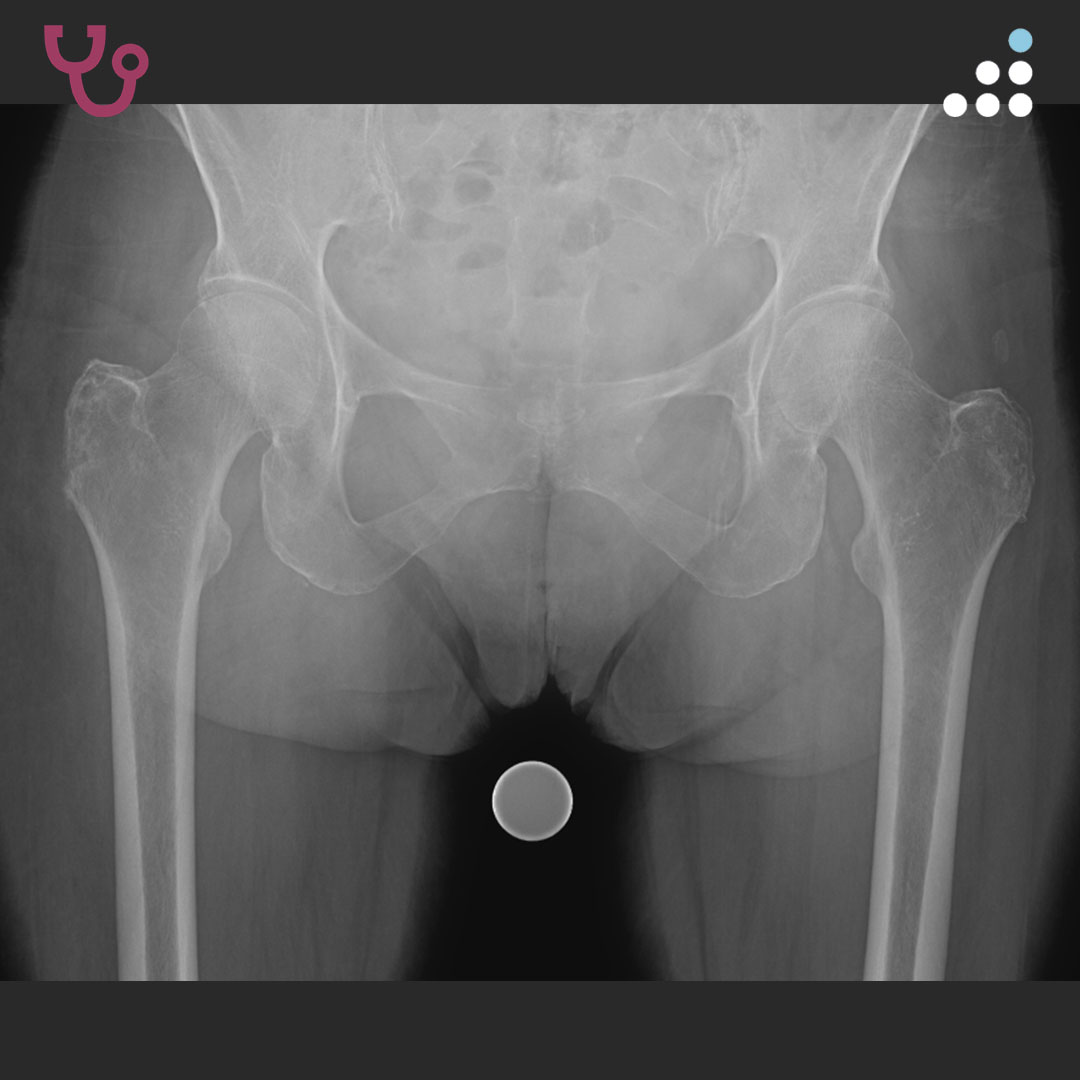
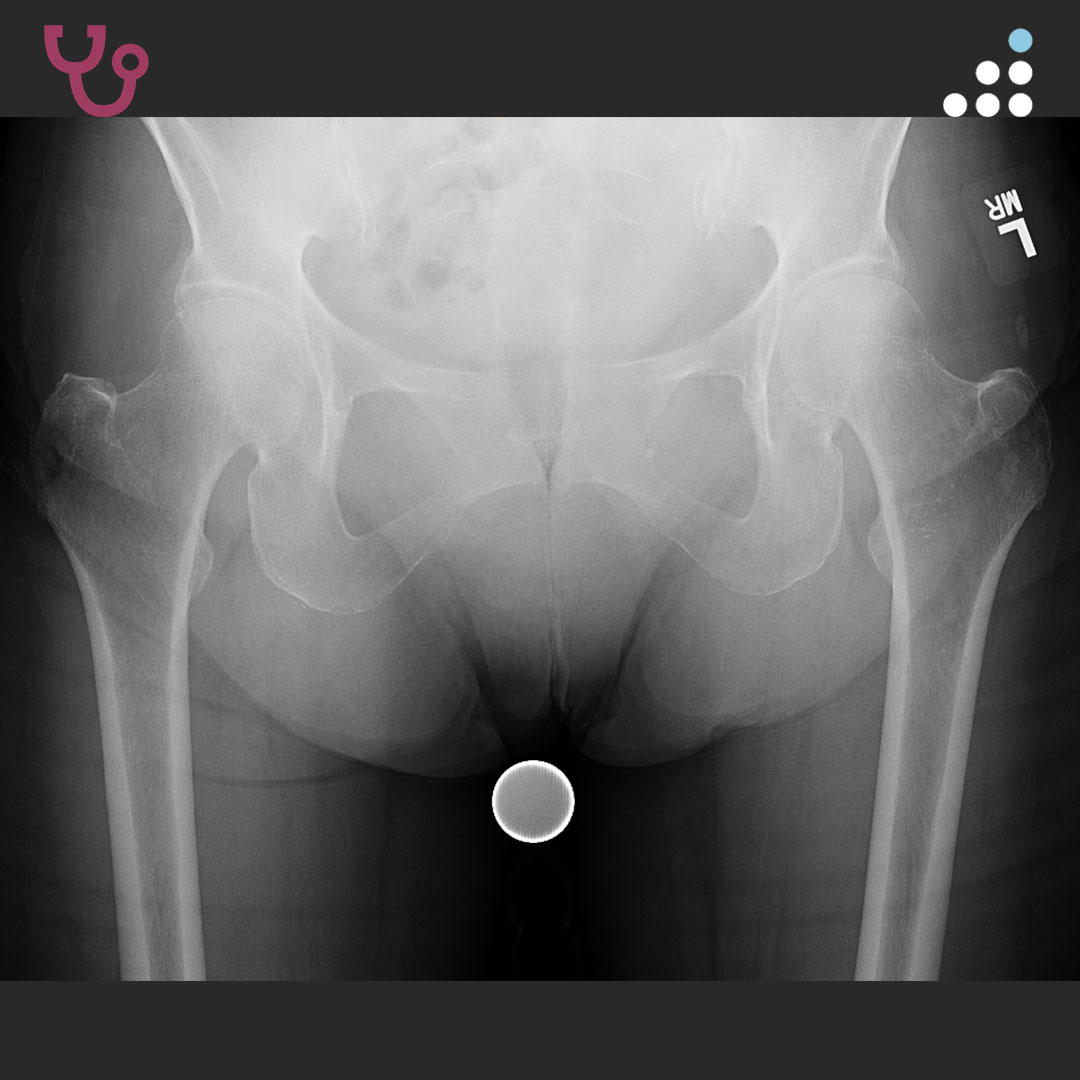
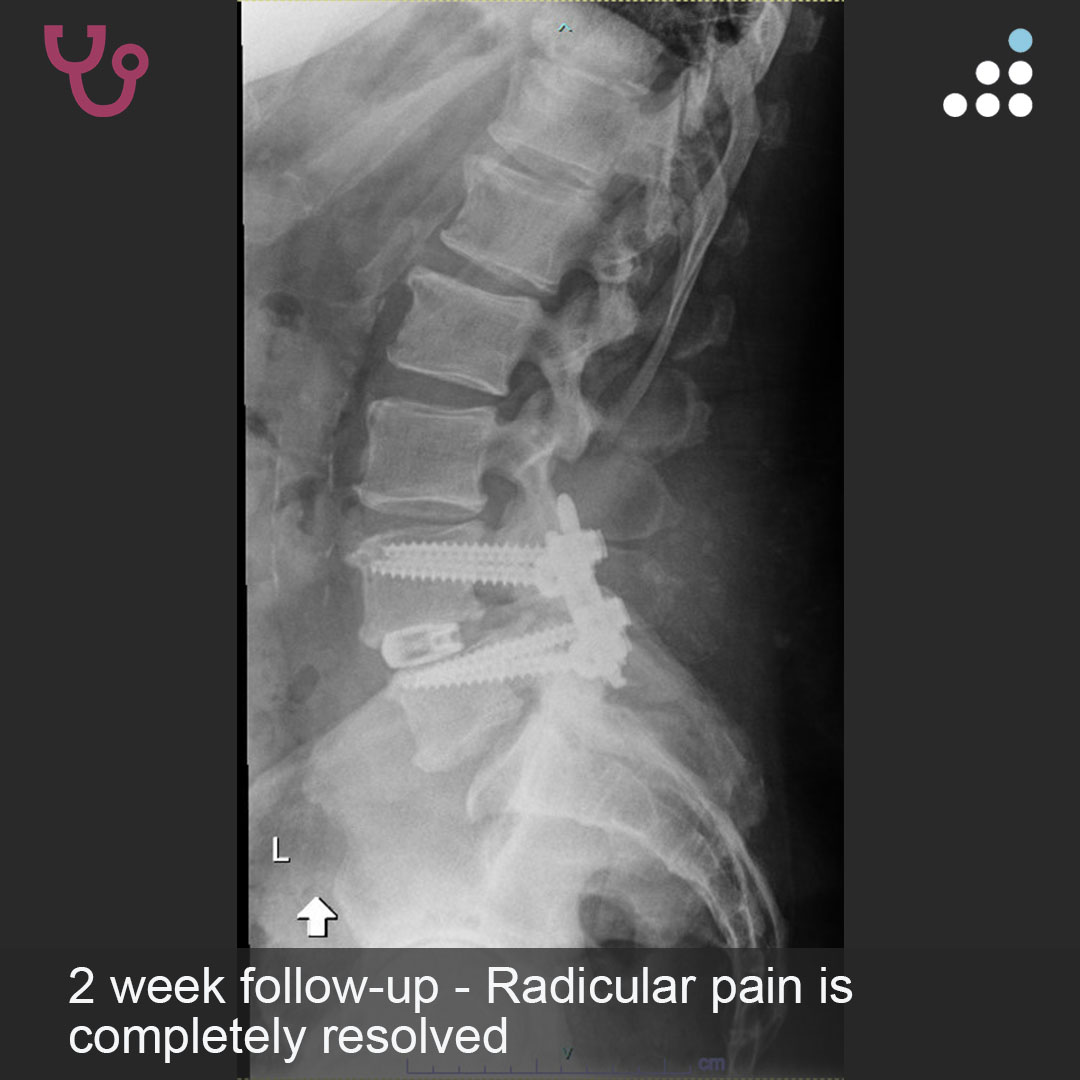
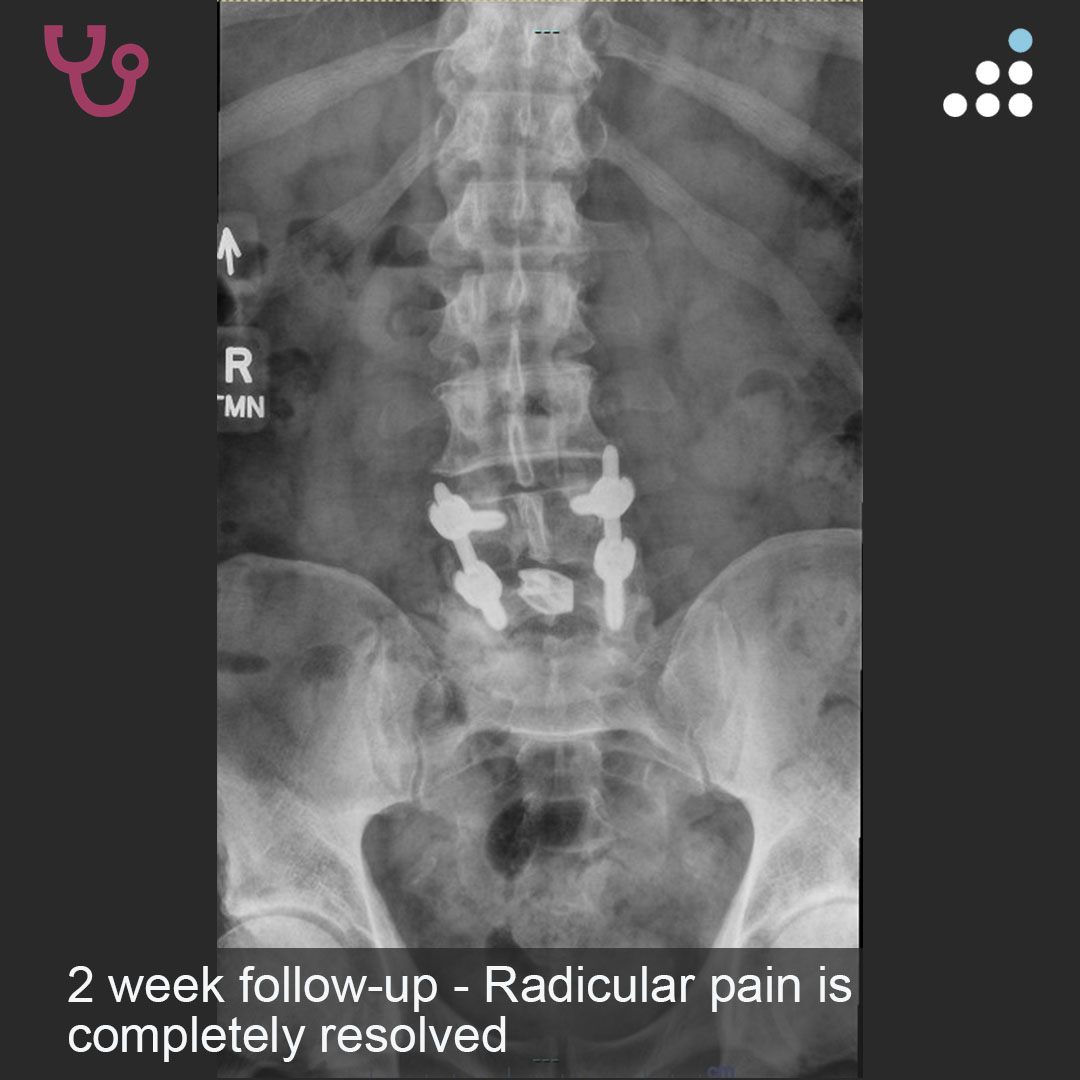
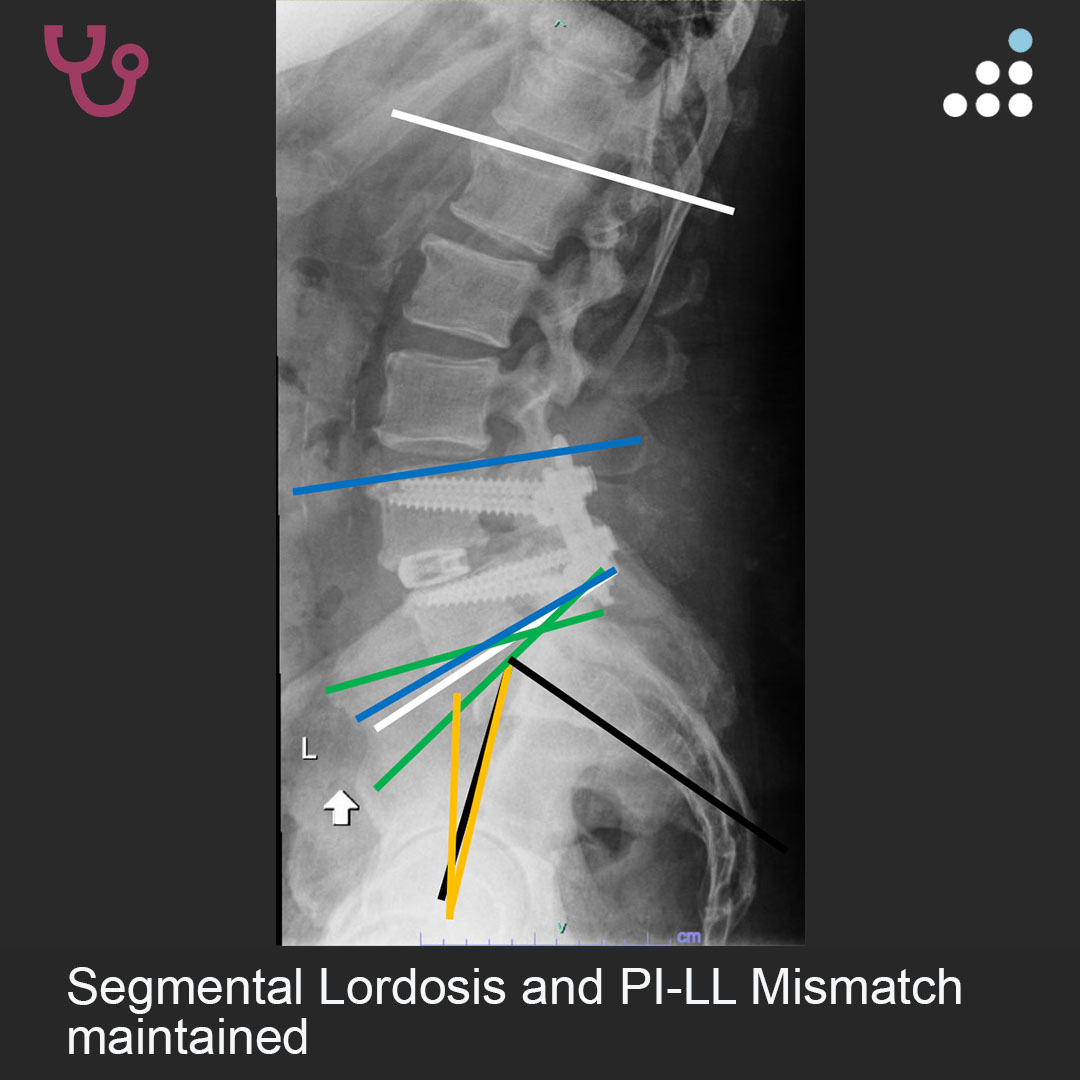
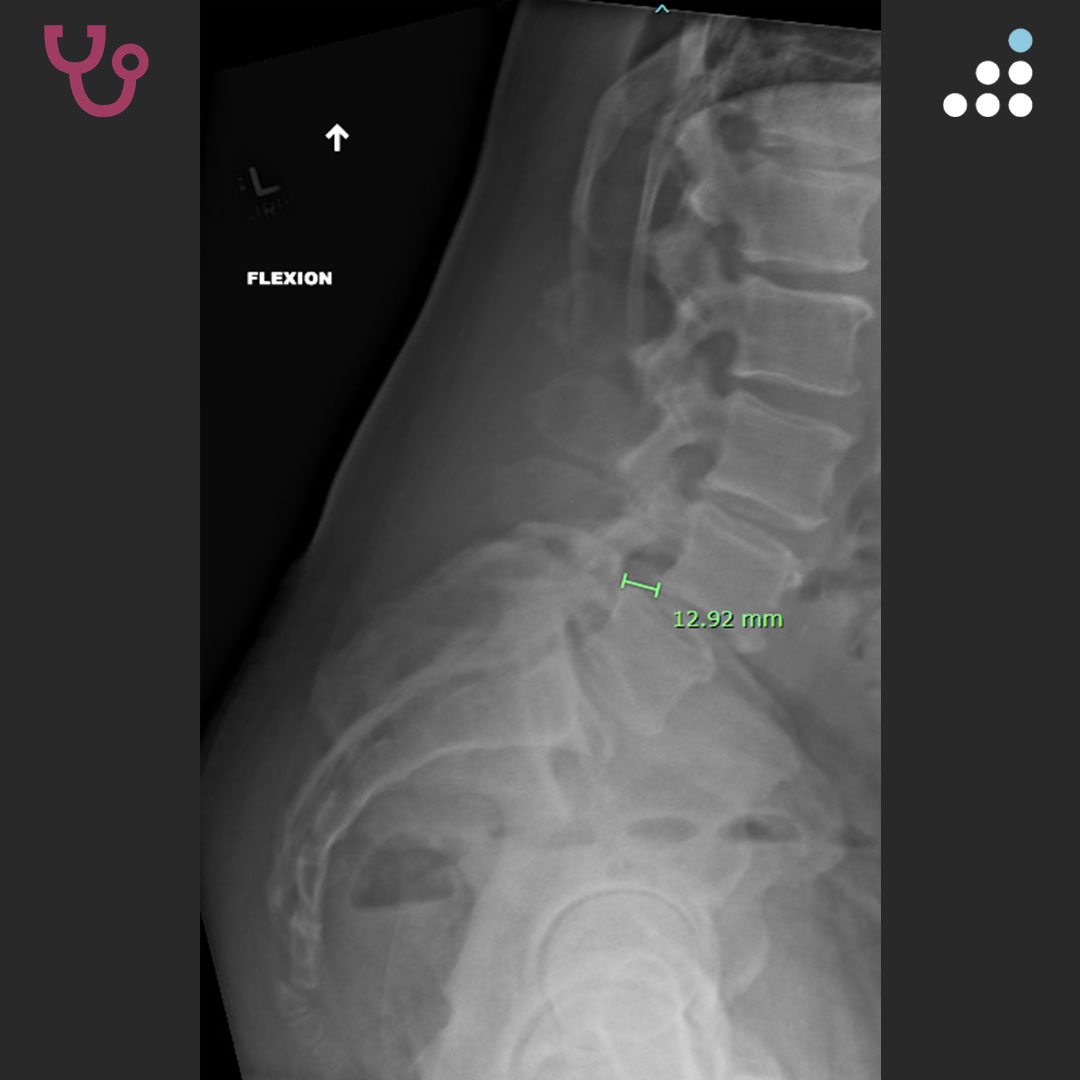
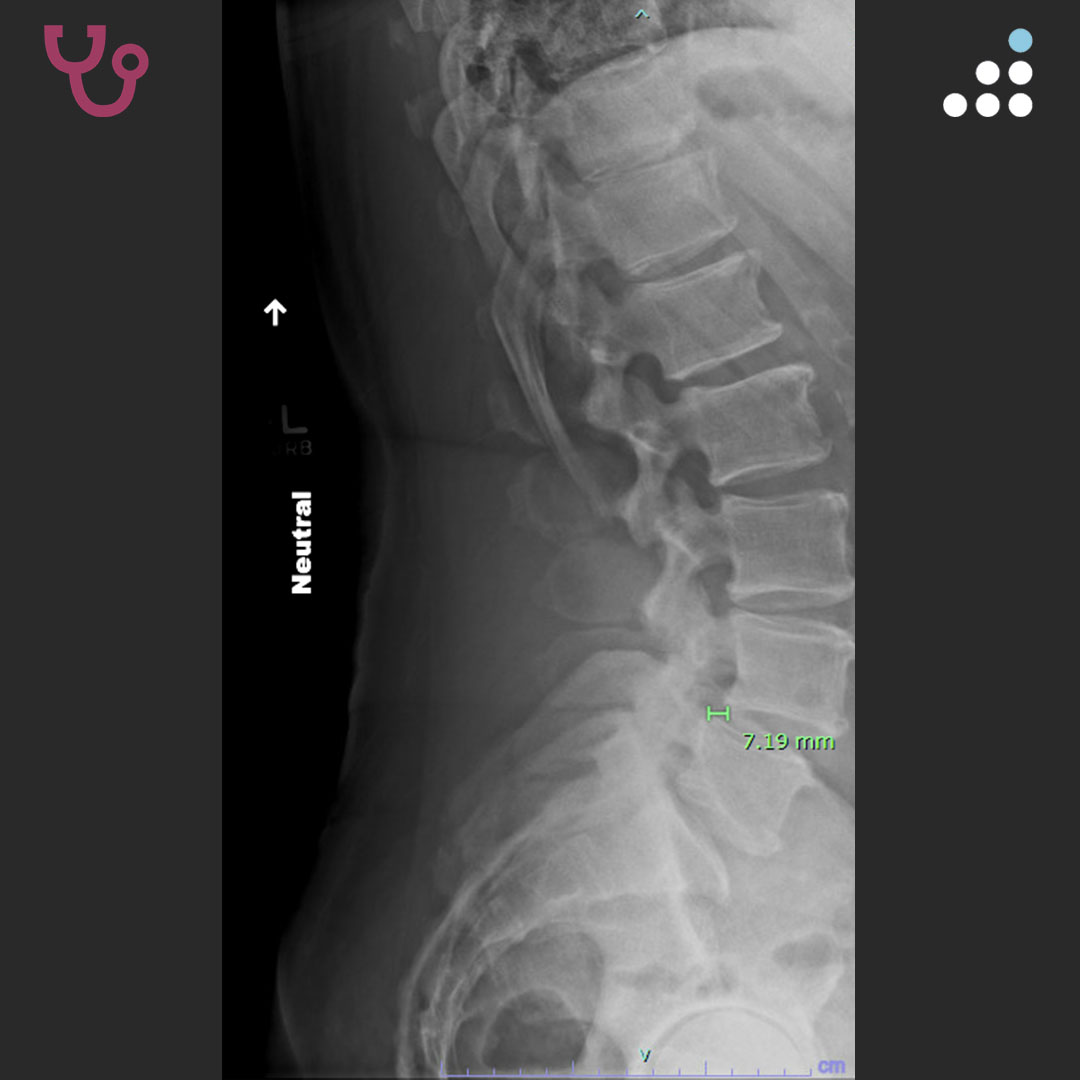
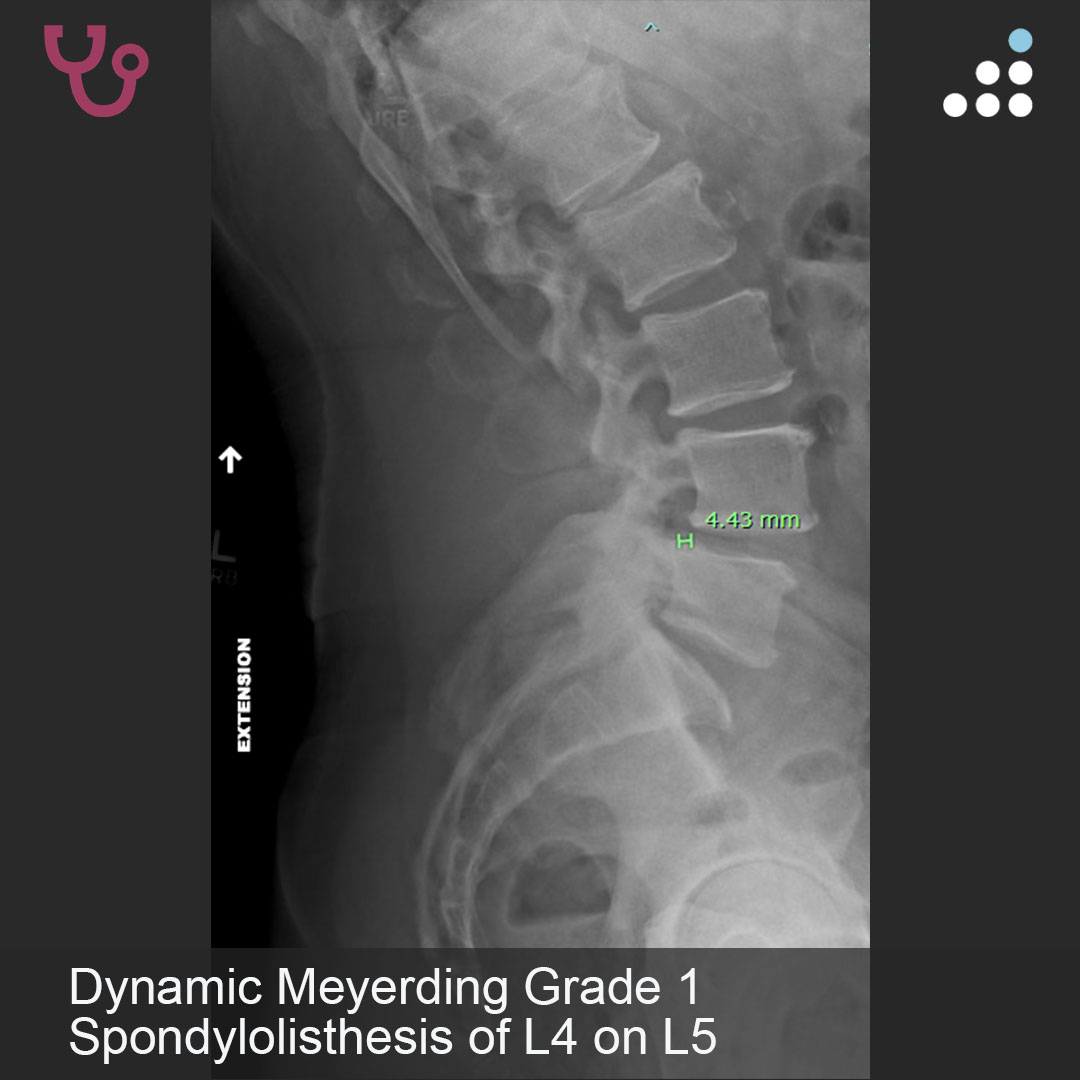
I wanted to see how good the AI is reading xrays. I uploaded this Xray and gave this prompt: What is the Anderson Orthopaedic Research Institute (AORI) Classification?
What do people think of the response.
Femur: AORI Type 1 – metaphyseal bone stock globally preserved, intact cortical rims, no large cavitary or segmental defects; long cemented stem not clearly bridging a major metaphyseal void.
Tibia: AORI Type 2A – proximal metaphyseal bone loss predominantly on one side with thinning/osteolysis, but overall cortical rim preserved and remaining metaphyseal bone capable of supporting a stemmed component.
Overall: AORI femur 1 / tibia 2A, based on AP view only; final classification subject to confirmation with lateral and intra-operative findings.
#orthotwitter, Would you agree with this assessment?

English