JP Mishra, MD, FACC
1.9K posts


JP Mishra, MD, FACC
@JPCardio
Upstate Cardiology. Rochester, NY. (seeking generosity, charity, friendship and passion for humanity).
















🚨 Endocrinology pearls you should never miss as a clinician 1️⃣ If you see elevated calcium, this is how you should think as a clinician? Most people remember “Stones, Bones, Groans & Psychiatric Overtones.” But that mnemonic doesn’t help you find the cause. What matters is a structured approach. When you see hypercalcemia, pause! think systematically. 🟢 FIRST RULE - CHECK PTH Your first lab is PTH. Don’t shotgun investigations. Don’t jump to imaging. PTH divides hypercalcemia into two diagnostic pathways. 🟢 INTERPRET THE PTH Only two possibilities: 🔻 PTH ↑ / inappropriately normal → PTH-mediated hypercalcemia 🔻 PTH ↓ → Non-PTH mediated hypercalcemia This single fork determines the entire work-up. 🟢 PATHWAY 1 : PTH HIGH → THINK PARATHYROID 🔴 Primary Hyperparathyroidism (Most common outpatient cause) Usually due to parathyroid adenoma (~85%). 🟢Mechanism :- PTH acts at three sites: 🔺Bone → osteoclast activation → calcium release 🔺Kidney → ↑ calcium reabsorption 🔺Kidney → ↑ vitamin D activation → ↑ gut absorption Net effect → persistent hypercalcemia. 🔻Typical Labs ↑ Calcium ↑ PTH ↓ Phosphate ↑ ALP ↑ Urinary calcium 🔻Why phosphate low? PTH causes phosphaturia by inhibiting Na-phosphate transporters in proximal tubule. 🔴 Familial Hypocalciuric Hypercalcemia (FHH) Mutation in calcium-sensing receptor. 🔻Typical Labs Mild ↑ Calcium Normal / mild ↑ PTH LOW urinary calcium ← key clue Normal phosphate Patients are asymptomatic → no surgery needed. 🔴 Tertiary Hyperparathyroidism Seen in long-standing CKD. Chronic stimulation → parathyroid glands become autonomous. 🔻Typical Labs ↑ Calcium ↑↑ PTH ↑ Phosphate ↓ Vitamin D 🟢 PATHWAY 2 :- PTH LOW → NON-PTH CAUSES If PTH is suppressed, calcium is coming from somewhere else. 🔴 Malignancy-Associated Hypercalcemia (Most common inpatient cause) Mechanisms: PTHrP secretion Osteolytic metastasis Excess vitamin D (lymphoma) 🔻Labs ↑ Calcium ↓ PTH ↑ PTHrP ↑ ALP 🔴 Multiple Myeloma Due to osteolytic bone destruction. 🔻Labs ↑ Calcium ↓ PTH ↑ ESR ↑ Total protein M-spike on SPEP CRAB C → Calcium R → Renal failure A → Anemia B → Bone lesions 🔴 Vitamin D Toxicity Usually from supplement overdose. 🔻Labs • ↑ Calcium • ↓ PTH • ↑ 25-OH Vitamin D • ↑ Phosphate 🔴 Granulomatous Diseases (Sarcoidosis, TB) Macrophages produce excess 1-α hydroxylase → ↑ active vitamin D. 🔻Labs ↑ Calcium ↓ PTH ↑ 1,25-OH Vitamin D ↑ ACE 🔴 Milk-Alkali Syndrome Excess calcium + absorbable alkali. Common sources: Calcium carbonate antacids Calcium supplements Calcium + vitamin D tablets Classic triad Hypercalcemia Metabolic alkalosis Renal dysfunction 🟢 CLINICAL CHEAT CODE If Calcium ↑ Step 1 → Check PTH PTH ↑ → Parathyroid causes PTH ↓ → Malignancy, Vitamin D excess, Granulomatous disease, Drugs One lab directs the entire diagnostic pathway. #MedTwitter #MedX #Endocrinology






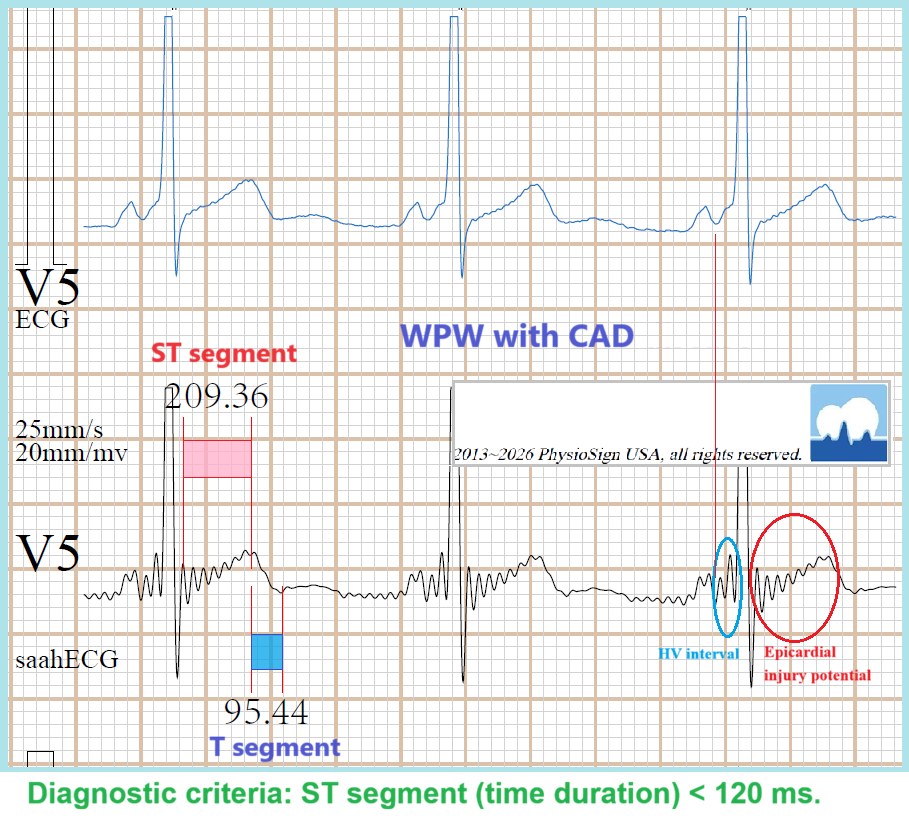
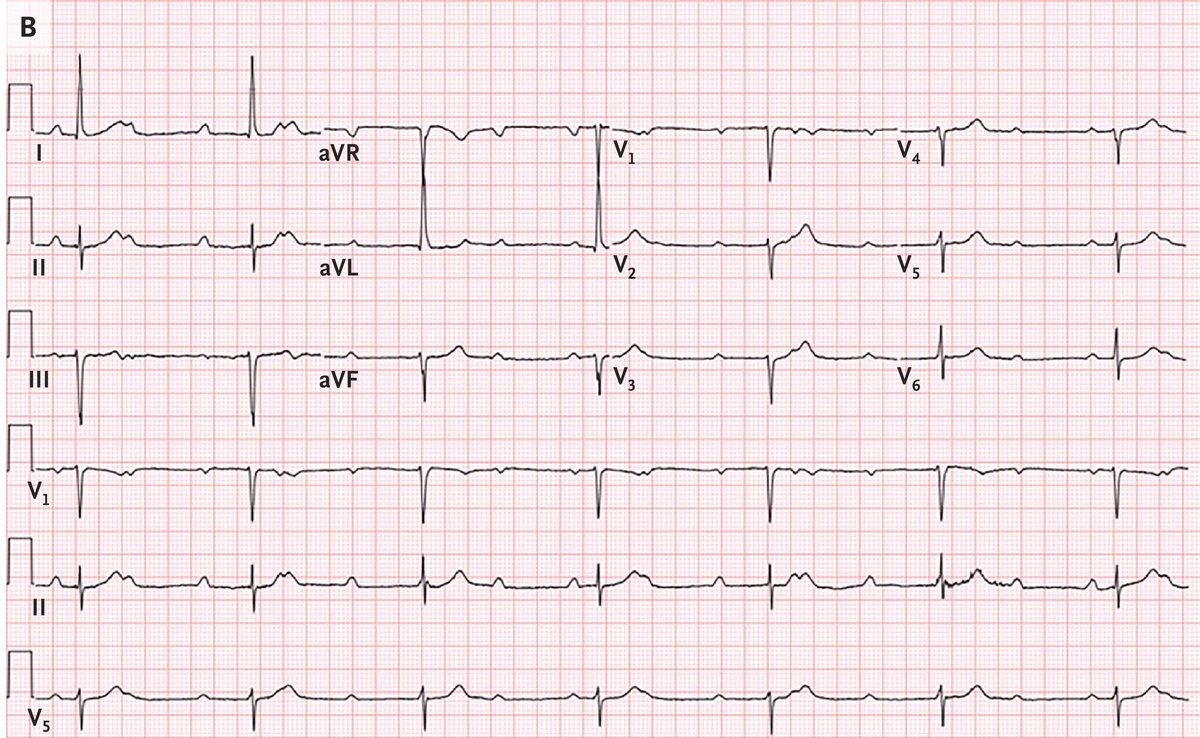
A 62 y/o male with chest discomfort. Thought ??






🚨Cardio-emergency pearls you should never miss as a clinician 7️⃣ In hypertensive crisis, the number misleads. The organs tell the real story lets break this down 🟥 HYPERTENSIVE EMERGENCY 🟨 SEVERE BP (NO ORGAN DAMAGE) 🔻1. Definition (Get this right first) Hypertensive crisis = BP ≥180/120 mmHg ⚠️ But classification depends on END-ORGAN DAMAGE, not the number: 🟥 Emergency → Acute target-organ injury 🟨 Severe BP → No injury 👉 Same BP. Completely different management. 🔻2. Terminology update 🟨 “Hypertensive urgency” → ❌ obsolete / discouraged 👉 Why? Misleading → overtreatment → harmful rapid BP lowering ✔️ Use: → Severe asymptomatic hypertension → Severe BP without organ damage 🔻3. Before labeling a crisis - verify BP. Pseudo-elevation is common. ✔️ Correct cuff size ✔️ Repeat after 5 min rest (seated, back supported) ✔️ Measure both arms (>15 mmHg difference → suspect vascular disease) ✔️ Check for: pain, anxiety, full bladder, recent caffeine/nicotine 👉 Many normalize → avoid unnecessary IV therapy 🔻4. Pathophysiology Chronic HTN → right-shifted autoregulation Acute rise → endothelial injury → fibrinoid necrosis + capillary leak → microangiopathy + ischemia Rapid BP fall → hypoperfusion → infarction 🔻5. Target Organ Damage (Defines EMERGENCY) 🧠 Neuro → encephalopathy, stroke, seizures ❤️ Cardiac → ACS, LV failure, pulmonary edema 🧂 Renal → AKI, hematuria/proteinuria 👁 Eye → papilledema, flame hemorrhages 🫀 Vascular → aortic dissection 🤰 Obstetric → preeclampsia/eclampsia 🔻6. MAP : what organs actually care about MAP = DBP + \frac{1}{3}(SBP - DBP) 👉 All targets are based on MAP reduction, not SBP alone. 🟨 SEVERE BP (NO ORGAN DAMAGE) 🔻7. Management (Do less, but do it right) ❌ No IV antihypertensives ❌ No rapid BP reduction ✔️ Start/adjust oral therapy ✔️ Identify triggers (pain, NSAIDs, steroids, non-adherence) ✔️ Reinforce compliance ✔️ Follow-up in 24–72 hrs ⚠️ Rapid lowering here → stroke / syncope risk 🟥 HYPERTENSIVE EMERGENCY 🔻8. Core principle - Controlled reduction: • 1st hour → ↓ MAP ≤25% • Next 2–6 hrs → ~160/100–110 mmHg (slight correction) • 24–48 hrs → gradual normalization ❌ Never normalize immediately 🔻9. Why this matters Chronic HTN → shifted autoregulation Rapid drop → hypoperfusion → → Stroke → MI → AKI 🔻10. Condition-specific targets 🫀 Aortic dissection → SBP <120 + HR <60 (within minutes) → IV beta-blocker FIRST (then vasodilator) 🧠 Ischemic stroke → No thrombolysis: allow ≤220/120 → Thrombolysis: Before: <185/110 After: <180/105 🧠 ICH → Target SBP ≈ 140 → Avoid <130 💦Pulmonary edema → IV nitroglycerin + diuretics 🤰 Preeclampsia/eclampsia → Labetalol / Hydralazine → MgSO₄ (seizure prophylaxis) sympathomimetic → ❌ Avoid pure β-blockers → Use benzodiazepines + vasodilators 🔻11. IV drugs (Know your weapons) ✔️ Nicardipine ✔️ Labetalol ✔️ Esmolol ✔️ Clevidipine ✔️ Nitroglycerin ⚠️ Nitroprusside → last resort (cyanide toxicity & sudden hypotension) 🔻12. Investigations (Don’t miss organ damage) 🧪 Labs: CBC, creatinine, electrolytes Troponin, LDH Urinalysis (protein/hematuria) Imaging: ECG CXR CT brain (if neuro signs) Echo (if cardiac involvement) 🔻BEDSIDE CLINICAL EXAM (MUST DO) General Mental status → encephalopathy? Seizures / confusion Vitals BP in BOTH arms Pulse deficit → Aortic dissection Eye (Fundoscopy) Papilledema → emergency Hemorrhages/exudates Cardiac S3 → LV failure New murmur → dissection (AR) Respiratory • Crackles → pulmonary edema Neuro • Focal deficits → stroke Peripheral • Weak/absent pulses → vascular cause 🔻14. Pitfalls (Exam + real life traps) ❌ Treating numbers blindly ❌ Overcorrection (>25% drop early) ❌ Missing aortic dissection ❌ Giving IV drugs in non-emergency ❌ Not doing fundoscopy #MedTwitter #MedX #Cardiology


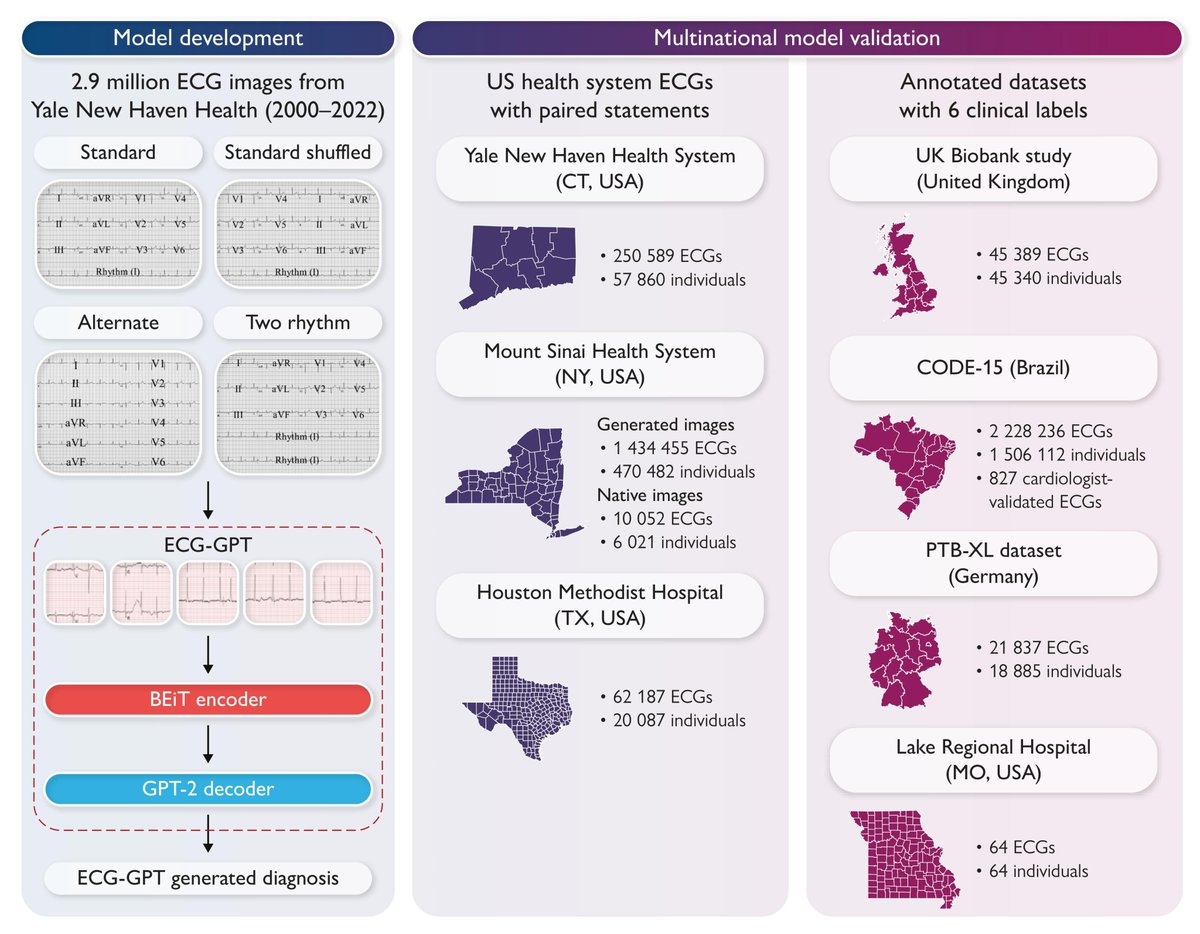



A 65-year-old man with severe chronic obstructive lung disease has been admitted to the intensive care unit for treatment of broncho-pneumonia. @dr_manish_ydv @Dr_Shiv_kumar_ @DrMedica_13 @drobiy12 @DrsansariOrd @hemo_shk @MiguelP23970914 @shakilED