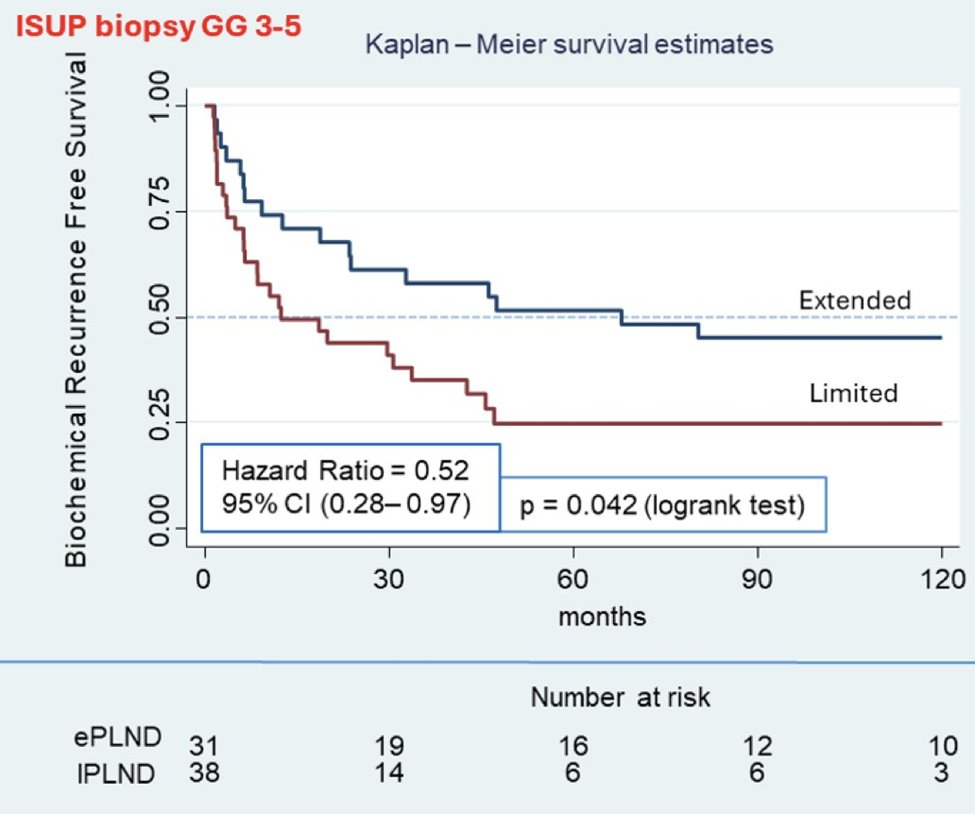
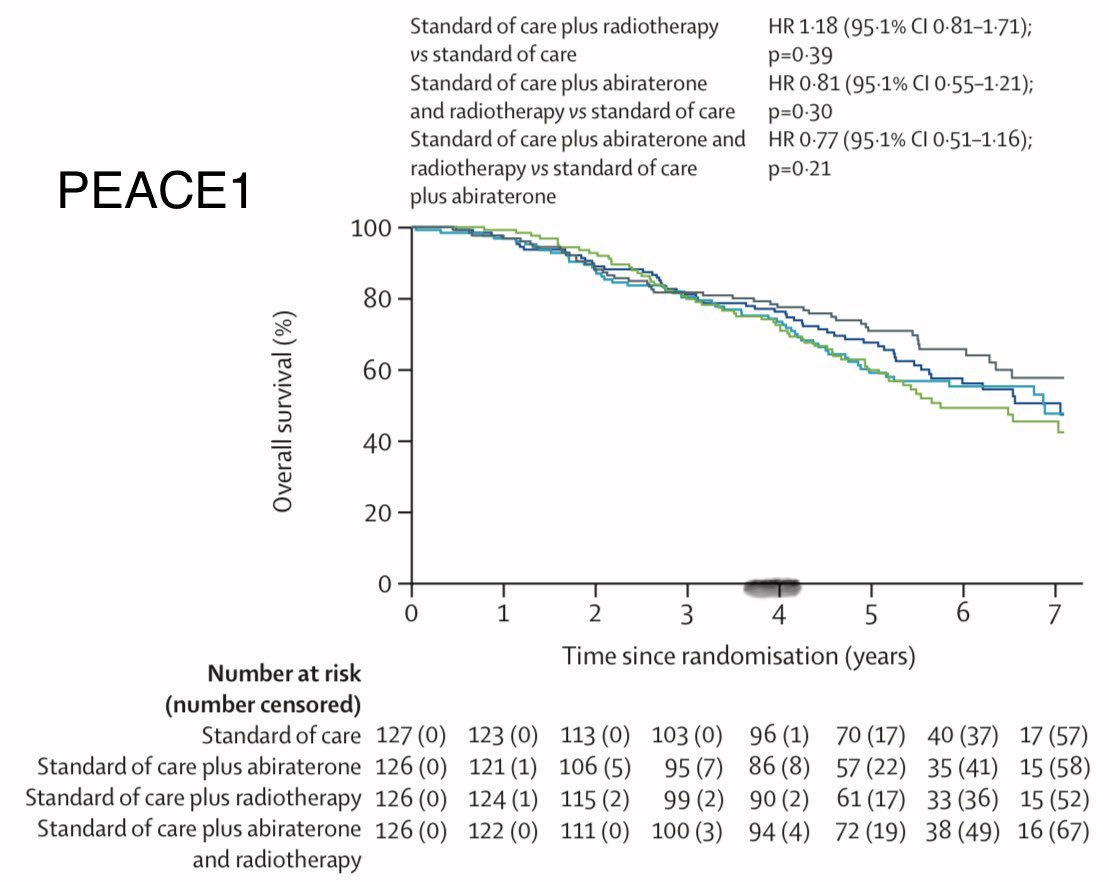
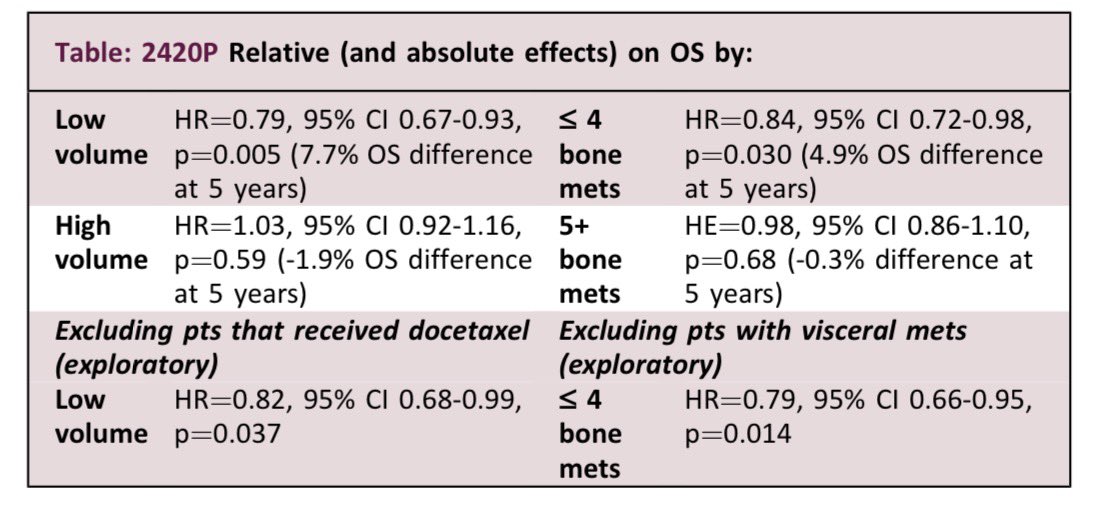
🚨The sequel is here!! The other 👞 drops. Cribriform morphology in ProtecT — now in prostatectomy specimens #ProstateCancer #radonc #UroSoMe @UroToday @APCCC_Lugano @PCF_Science @OncoAlert 🧵1️⃣
Tony Felefly
1.1K posts


@TonyFelefly
Radiation Oncologist | MSc Physics | PhD AI & Quantum Computing / Oncologic Imaging | Views are my own

🚨The sequel is here!! The other 👞 drops. Cribriform morphology in ProtecT — now in prostatectomy specimens #ProstateCancer #radonc #UroSoMe @UroToday @APCCC_Lugano @PCF_Science @OncoAlert 🧵1️⃣



Waiting for @TylerSbrt7 to unpack this in a 🧵 Thanks to the ProtecT trial team, the great pathologists who conducted the review, the OCHRe and CUH Tissue Bank teams who retrieved and digitised slides, and all trial participants @Freddie_Hamdy @Tristan_Radiol @ian263









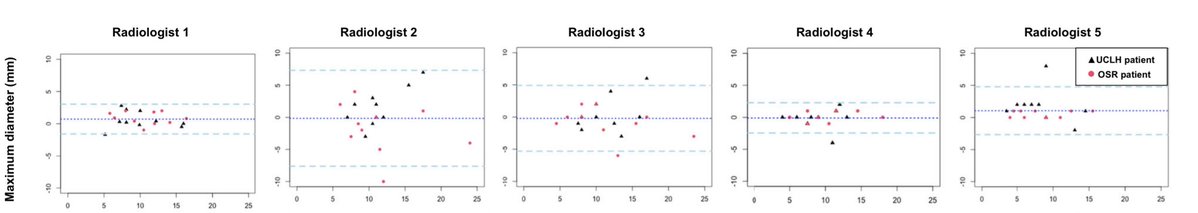











PRESIDENT Trial: Can RP improve outcomes in LV mHSPC? #EAU26 @urotoday RCT testing RP + systemic Rx vs systemic Rx alone in PSMA PET LV mHSPC (n=749) Primary EP: Deterioration-FS (HRQoL decline, metastatic progression, or death) Trial opens 2026 across 26 🇬🇧 sites

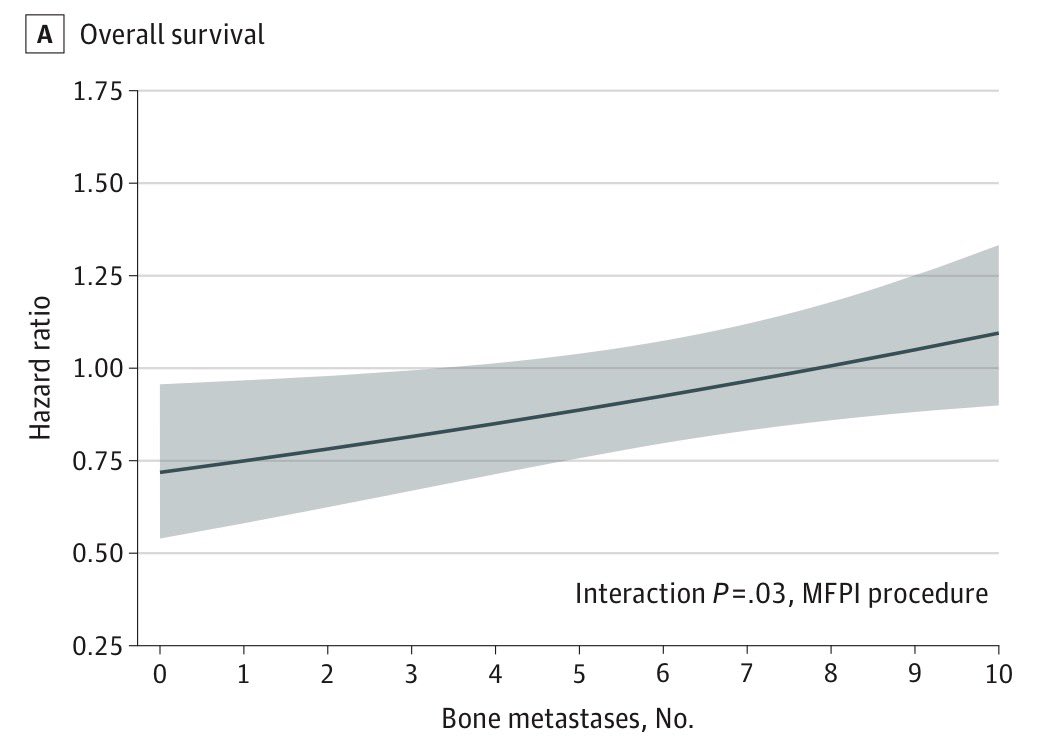


Lutectomy not really looking like an interesting option. Back to the drawing board I guess? @declangmurphy

Modern prostate cancer care is about intensity and timing. ADT + ARPI is the foundation. We then add radiation or chemo based on the individual. @APCCC_Lugano @Uroweb #EAU26



📣@ChapinMD presents best systemic therapy trial +/- prostatectomy n=120 randomised phase II trial in #prostatecancer. No observed benefit for prostatectomy 🔪🩸. Ongoing recruitment for SWOG-1802, pls support this important clinical trial 👏🏽#pcsm #EAU26