

cardio Roland
922 posts

@CardioRoland
It’s all about flow! heart failure, biomarkers and aorta cardiologist, suffering from cardioglossopexia (hart op de tong) tweets on personal title








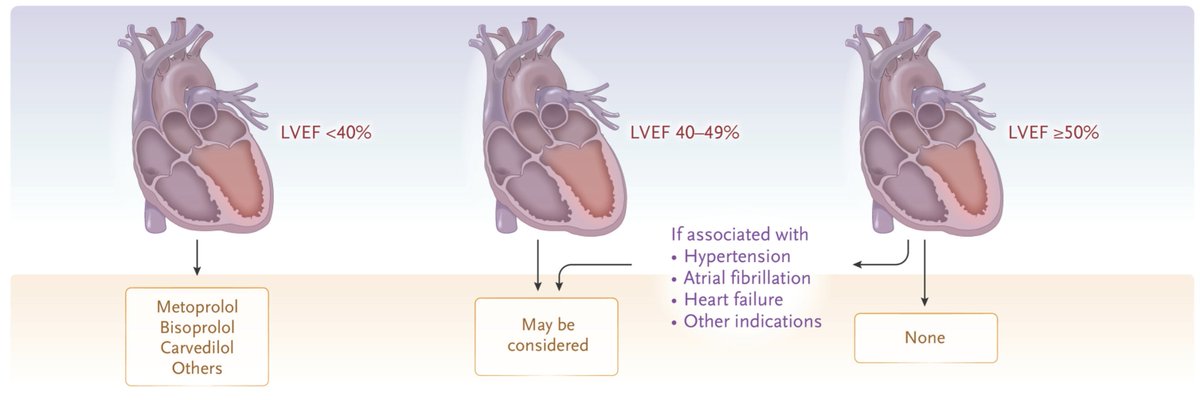










No benefit from beta-blockers in patients with recent myocardial infarction and LVEF equal or greater than 50%. #AHA2025 IPD meta-analysis of 5 RCTs including 17,801 patients (REBOOT, REDUCE-AMI, BETAMI, DANBLOCK, and CAPITAL-RCT). @Borjaibanez1 @dan_atar @RosselloXavier @evaprescott @drjohnm @mmamas1973 @djc795 @mirvatalasnag @EAPCIPresident @SABOURETCardio @Hragy @kaulcsmc @EricSecemskyMD @venkmurthy @DrMarthaGulati @SripalBangalore @sbrugaletta @DLBHATTMD @EricTopol @CMichaelGibson @DFCapodanno @nadig_cardio @Ortega_Paz @HadyLichaaMD @ACCinTouch @Medscape @AHAScience Published on @NEJM nejm.org/doi/full/10.10…








Wow, the game has changed! #SURPASSCVOT meets its primary & secondary endpoints in first *head-to-head* CV outcomes trial! Tirzepatide (dual GLP1/GIP agonist) vs Dulaglutide (GLP-1RA) including 16% lower risk of all cause mortality! investor.lilly.com/news-releases/…