Sabitlenmiş Tweet

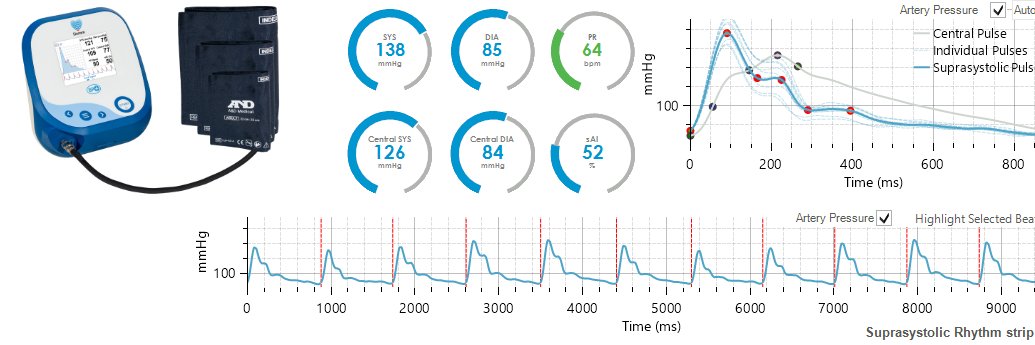
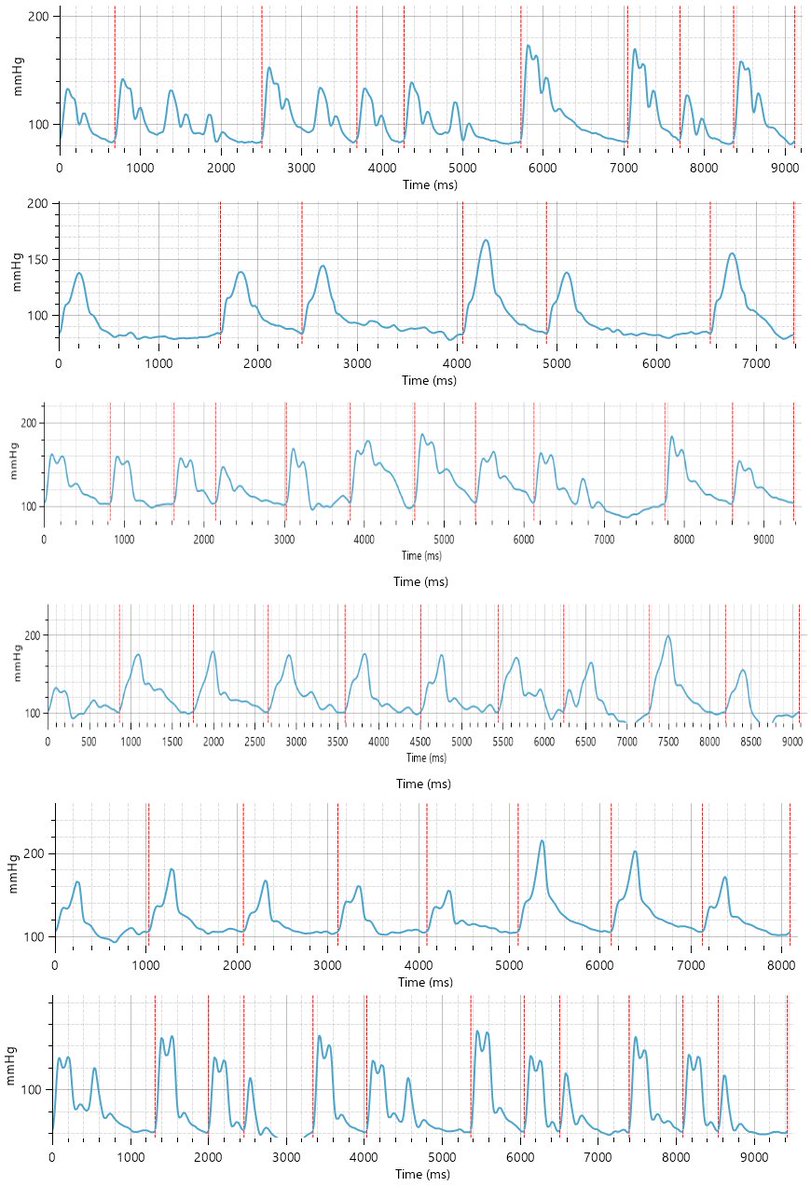
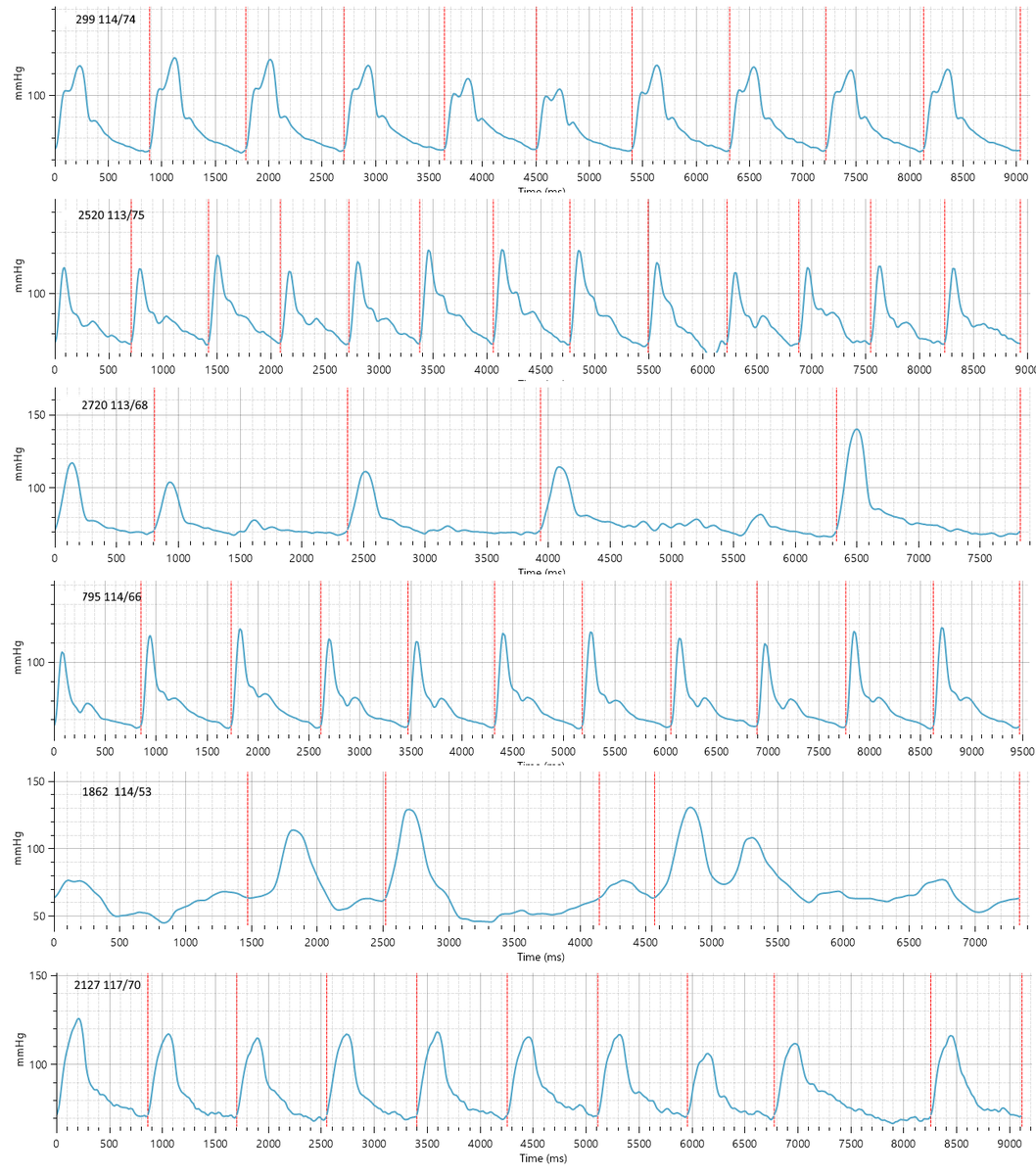
@JohnRMontford @kramer_holly Non-invasive measurements using a regular upper-arm cuff can accurately measure intra-arterial waveforms, including people with bad vascular disease without risks associated with an invasive measurement!
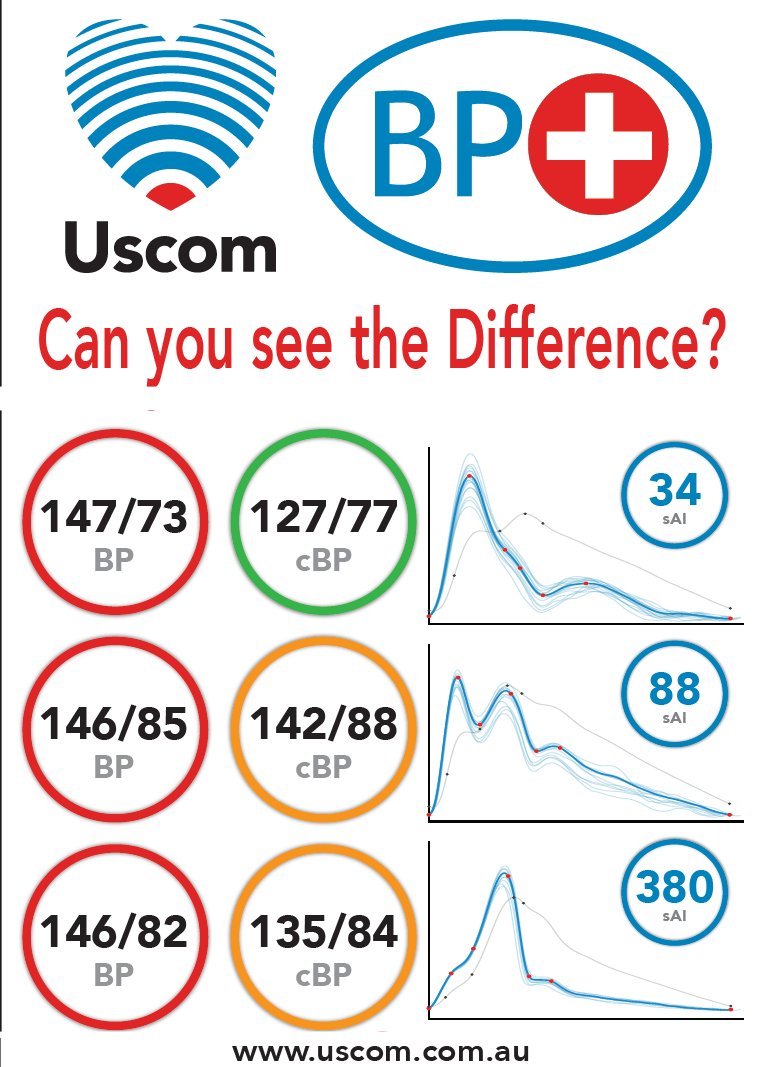
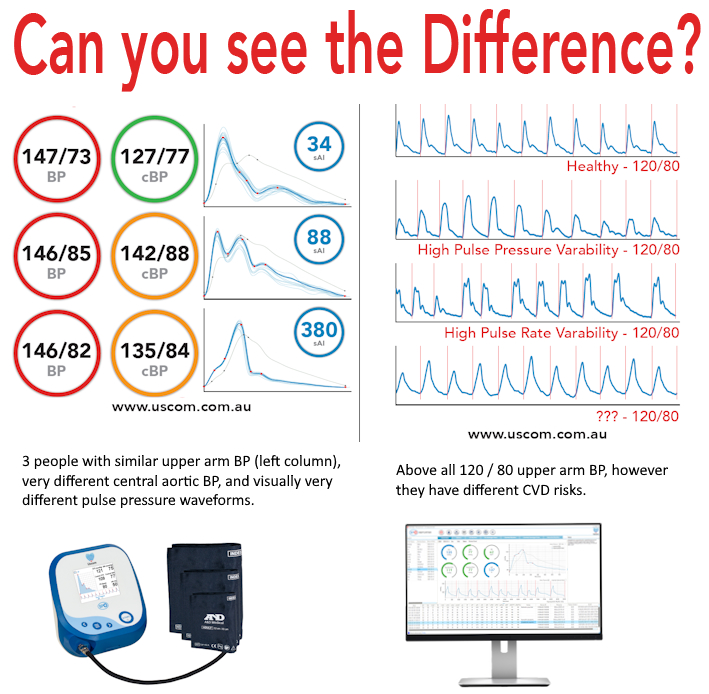
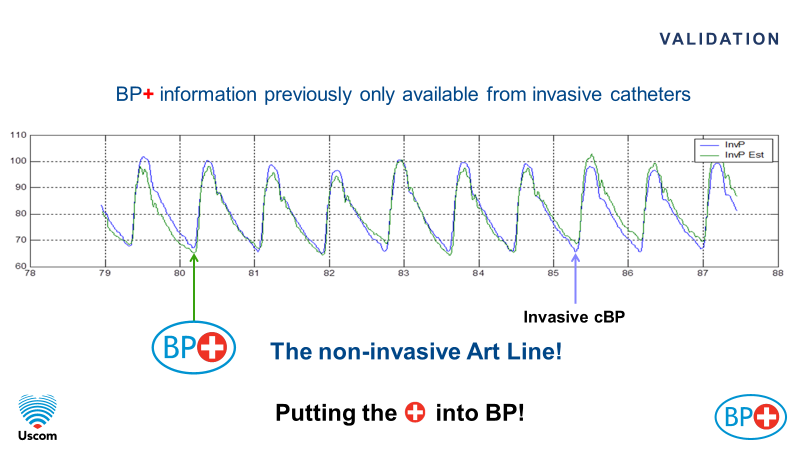
Blue = invasive aortic catheter
Green = calculated aortic waveform
English