
Simon Dankel
2.1K posts

Simon Dankel
@simondankel
Professor/Scientist (Medicine, Physiology, Metabolism, Molecular Biology, Genomics), Nutritionist, Food Engineer, husband of @dorothydankel, father of 3 girls




🚨🚨🚨🚨🚨🚨🚨🚨 Match Analysis Paper Now Published! jacc.org/doi/10.1016/j.… 🙏🙏Please RT far and wide 🙏🙏 KETO-CTA (#LMHRstudy) vs Matched Controls (#MiHeart) METHODS – 80 participants from the #LMHRstudy were matched 1:1 with asymptomatic subjects from #MiHeart, considering age, gender, race, diabetes, hyperlipidemia, hypertension, and smoking history. PRIMARY ANALYSIS – High-resolution heart scans (#CCTA) were used for evaluating Total Plaque Score (TPS), Total Stenosis Score (TSS), and Segment Involvement Score (SIS). RESULTS Matched mean age: 55.5 years, with average #LDL cholesterol of 272 mg/dL (max LDL-C of 591 mg/dL) after an average of 4.7 years on a ketogenic diet. 🚨 There was no significant difference in coronary plaque burden between the #LMHRstudy group (mean LDL-C 272) and #MiHeart controls (mean LDL-C 123 mg/dL); note: pre-KETO LDL-C in the KETO group was 122 mg/dL. 🚨 No significant difference in CAC (median and IQR) [0 (0, 56)] vs [1 (0, 49)], p = 0.520. 🚨 No correlation between elevated LDL-C and plaque levels. ⚠️ NOTE: This analysis focuses on baseline scans. More data will follow from the Keto-CTA longitudinal study in the coming months. Please continue to consult your healthcare provider. 🙏🙏🙏 A huge thank you to everyone who made this milestone publication possible. 🙏🙏🙏 Special shout-out to @nicknorwitz, @DrRagnar, @AdrianSotoMota, @khurramn1, and of course, @BudoffMd. And a MASSIVE thanks to all who contributed their time, money, and support to help make this research a reality! (PS — This is Open Access -- so you are free to download and read in its entirety)

👉Atherosclerosis IS NOT an Inflammatory disease ☝️Atherosclerosis is not fundamentally an inflammatory disease; rather, it is primarily a disorder characterized by the penetration and retention of apolipoprotein B (ApoB) in the subendothelial space. The process begins when ApoB-containing lipoproteins enter the endothelial layer, subsequently becoming retained and modified. This sets the stage for an inflammatory reaction that intensifies the atherosclerotic process. Similar to how COVID-19 involves an important inflammatory component in its development but is caused by the SARS-CoV-2 virus—addressed with vaccines—atherosclerosis also features a critical inflammatory aspect. However, its primary trigger is the accumulation of ApoB. Therefore, treatment strategies should focus on reducing ApoB levels and concurrently managing the inflammatory response to effectively curb the progression of atherosclerosis. This approach aims at addressing the root causes of the condition, offering a more direct and potentially effective method of treatment.








In this review, the outcome measures in the unprocessed/ultra-processed by @KevinH_PhD were assessed as "high risk of bias", resulting in low "certainty of evidence" e.g. for reduction in energy intake in this trial. Seems very strange to me. pubmed.ncbi.nlm.nih.gov/38988861/

Is "overeating" the cause or consequence of getting fat? Human studies are too short to provide an answer. So we reviewed the animal research. 👉In almost every case, evidence shows an underlying metabolic problem driving the positive energy balance #CIM onlinelibrary.wiley.com/doi/10.1111/ob…




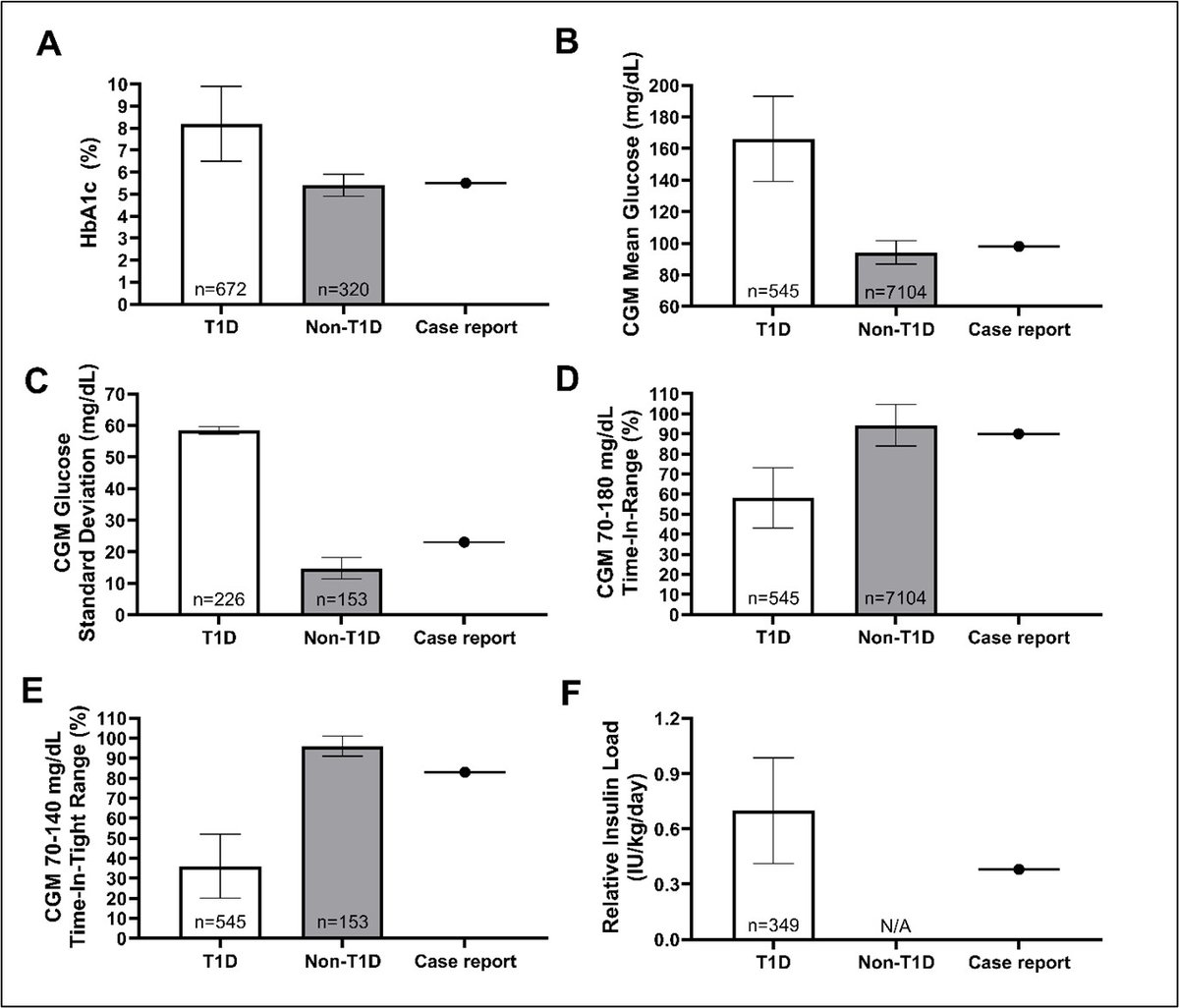
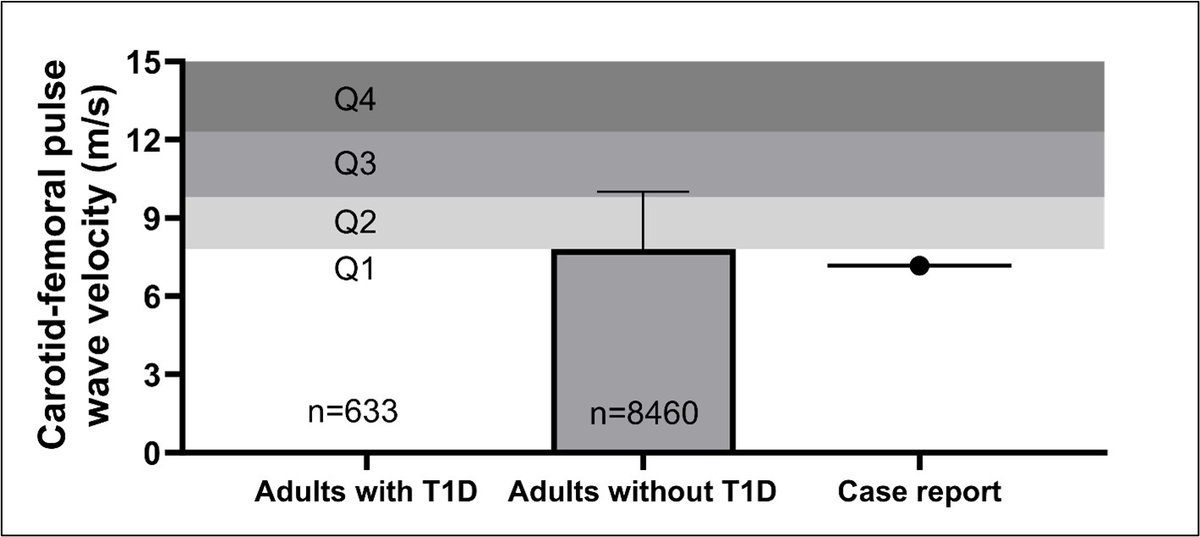
🔬🤯🫀 10-Years longitudinal data on KETOGENIC DIET and Safety, Efficacy & Advanced Cardiovascular Physiology in a patient with HIGH RISK cardiovascular disease (Type 1 Diabetes)? #ADA2024 NEW DATA OUT TODAY: journals.physiology.org/doi/abs/10.115… We (@Joseph_Watso) measured advanced cardiovascular health profile in an adult with elevated cardiovascular risk (type 1 diabetes) who followed a ketogenic diet for 10 years and sustained euglycemia (10-Year HbA1c 5.5%)...what did we find? Was it safe? Did it progress early signs of cardiovascular disease? 1) CLINICAL IMPORTANCE: People with type 1 diabetes (T1D) show early artery damage within 4 years, estimated 10x higher risk of heart disease and 11-18 year early death...Hyperglycemia, as well as insulin, lipids, etc... are believed to drive this risk...the ketogenic diet has been proposed as a promising strategy...but people have concerns about long-term CV risk of KD. 🤯NOTE: THIS IS ONE OF THE LONGEST CONFIRMED REPORT OF KD AND IS THE LONGEST LONGITUDINAL REPORT OF A PATIENT WITH TYPE 1 DIABETES FOLLOWING A KETOGENIC DIET IN THE LITERATURE. 🔬 2) METHODS: VERY UNIQUE case of a patient at high risk for CV disease (type 1 diabetes) who MAINTAINED body composition (DXA confirmed), activity, and calories over a 10-year period (confirmed elevation of R-BHB) while following a KD. Why is this important? Removing confounding influence of body composition, physical activity, and caloric changes allows us to look at macronutrient specific effects of a KD. To our knowledge there is no long-term report where these were controlled...let alone over 10 years in an at risk population allowing us to more closely look at CV impact of KD. 🩸📉3) GLUCOSE & INSULIN RESULTS (1/6): During a 60-day CGM tracking period, the participant demonstrated excellent glycemia (10year HbA1c: 5.5%), achieving mean blood glucose (98mg/dL), glycemic stability, and time-in-range in the top 1 percentile and total insulin load in the top 10 percentile compared with age/sex-matched patients with T1D. 🩸📈4) LIPID RESULTS (2/6): Although LDL-C was elevated over 10-year period on KD, most standard lipid values were not outside normal ranges. Advanced lipid testing demonstrated that LDL-C composition was Pattern A, borderline-high Apolipoprotein B (96mg/dL) and LDL-P (1415nmol/L), consistent with elevated LDL-C; however, Lipoprotein (a) (18.7nmol/L), small LDL-P (<90 nmol/L), LDL size (21.9 nm), and Lp-PLA2 Activity (182 nmol/min/mL) were all within the target range. WHAT ABOUT EARLY SIGNS OF CARDIOVASCULAR DISEASE PROGRESSION WITH 10-YEAR ELEVATED LDL-C? LETS SEE: 🫀🩸 5) STIFFNESS OF ARTERIES & BLOOD PRESSURE: Central artery stiffness (i.e., cf-PWV) was in the lowest (i.e., best) quartile for adults with T1D and similar to adults without T1D. The value of 7.17 m/s was 0.93 m/s lower (i.e., better) than the age-predicted cf-PWV of 8.10 m/s despite the presence of T1D. Not pictured - Seated office BP was 113/67 mmHg during an annual exam (systolic: 18th percentile for T1D; diastolic: 12th percentile for T1D) and ambulatory awake BP was 132 ± 15 mmHg for systolic BP and 80 ± 6 mmHg for diastolic BP. 6) ENDOTHELIAL FUNCTION: A) The peak blood flow response after ischemia (i.e., hyperemic velocity time integral) value was in the third quartile (50-75th percentile, 2nd to best group) of risk from adults without T1D. B) The blood vessel relaxation after ischemia (i.e., flow-mediated dilation, gold-standard assessment of vascular endothelial function) was higher (i.e., better) than adults with and without T1D. ⚡️7) AUTONOMIC REGULATION: The ability to modulate heart rate to maintain blood pressure (i.e., cardiac vagal baroreflex gain) was higher (i.e., better) than adults with and without T1D. Not pictured - Resting heart rate was below (i.e., better) than adults with and without T1D, SDNN (a common HRV marker) was similar to adults with and without T1D, and the Low-Frequency/High-Frequency HRV ratio was lower (i.e., greater parasympathetic dominance) than adults with and without T1D. 🫀 8) LEFT VENTRICULAR FUNCTION: There was no indication of left ventricular diastolic dysfunction. Not pictured - The participant presented with normal sinus rhythms with no sign of Q-T prolongation. 🚨⚠️9) LIMITATIONS: There are clearly limitations, primarily that this is an individual case. However, due to the sheer absence of long-term data, hypothesized risk of a KD, and popularity and use of KD, this data is important to share to generate future research questions. 🗒️CONCLUSION: In the longest known longitudinal report of a ketogenic diet in a patient at high risk for cardiovascular disease (type 1 diabetes), we observed that a KD could be a promising therapeutic option for managing cardiovascular disease risk when combined with other health behaviors. These initial findings should provoke further research into interventions like ketogenic diets to reduce the long-term health risks faced by those living with T1D while closely monitoring both traditional and advanced cardiovascular risk markers. Especially considering that currently available therapies do no reliably allow patients to achieve <7% HbA1c, let alone <5.7% HbA1c. 🔍MORE DATA: YES, MORE IS COMING. 10-YEAR SAFETY AND EFFICACY DATA ON 🦴BONE MINERAL DENSITY, 🚨THYROID FUNCTION, 🚨KIDNEY FUNCTION, & ⚠️LONG TERM CLINICAL ADVERE EVENTS OF A KETOGENIC DIET WILL BE PRESENTED SHORTLY. STAY TUNED... @Joseph_Watso CV & Applied Physiology Lab caplaboratory.com Study how health behaviors (e.g., diet, exercise, etc.) affect cardiovascular health and physiology @SansumDiabetes sansum.org Studying how lifestyle, tools, and medicine affect people with diabetes. TEAM: @AusRob_PhD @sa01singar @fsucehhs @FSUResearch @FSUISSM @AJPCellPhys @diaTribeNews @BeyondType1 @MCRiddell1







Ultra-processed food corporation power is growing, & multi-stakeholderism is broadly accepted in global food governance. But who governs powerful multi-stakeholder institutions and what are their implications for UPF policy responses, governance & food system transformation? 👇🏼


