
Tom Hyde
2.3K posts


@CotsCardiology
Cardiologist with an interest in coronary artery disease, from prevention to stenting. Professional account, views my own. Occasionally misunderstood.
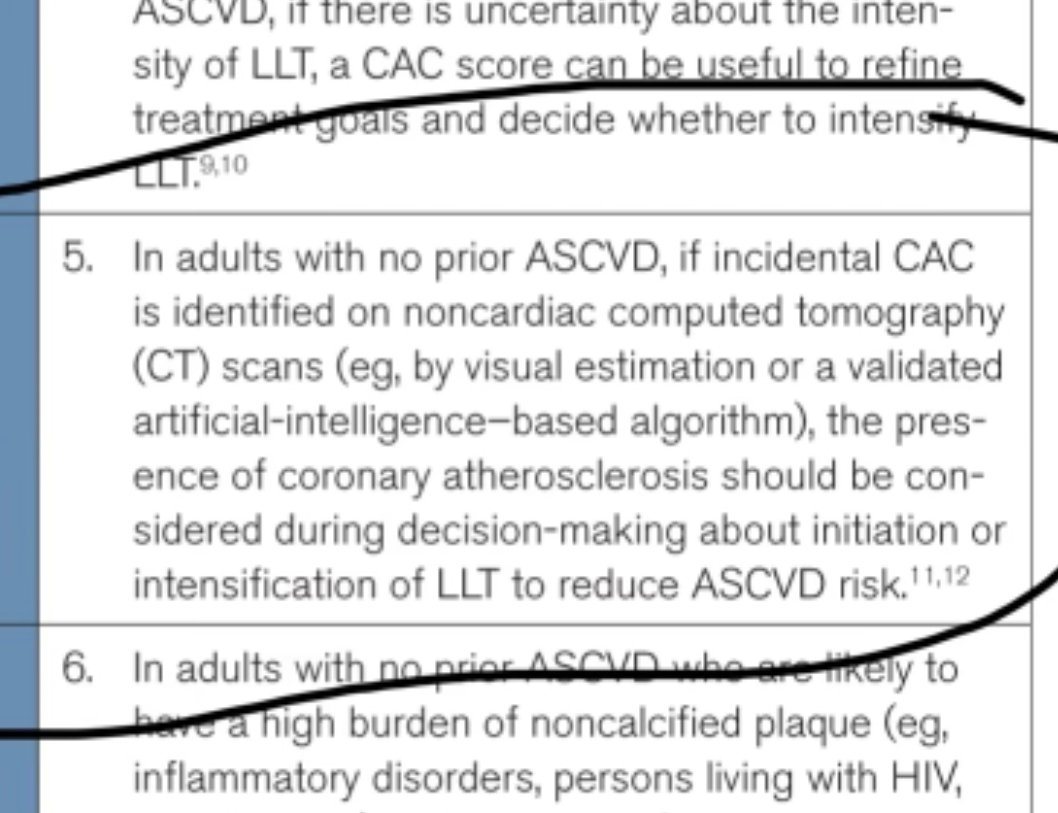






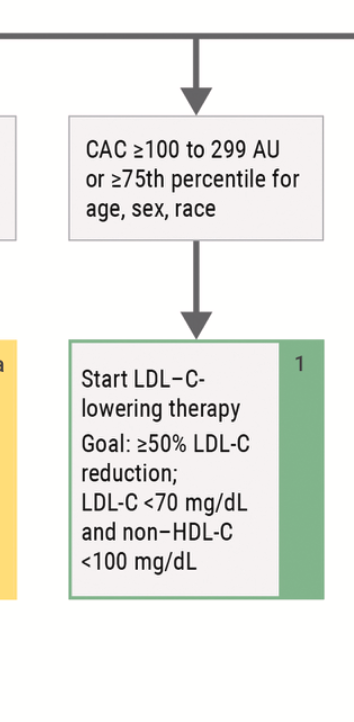
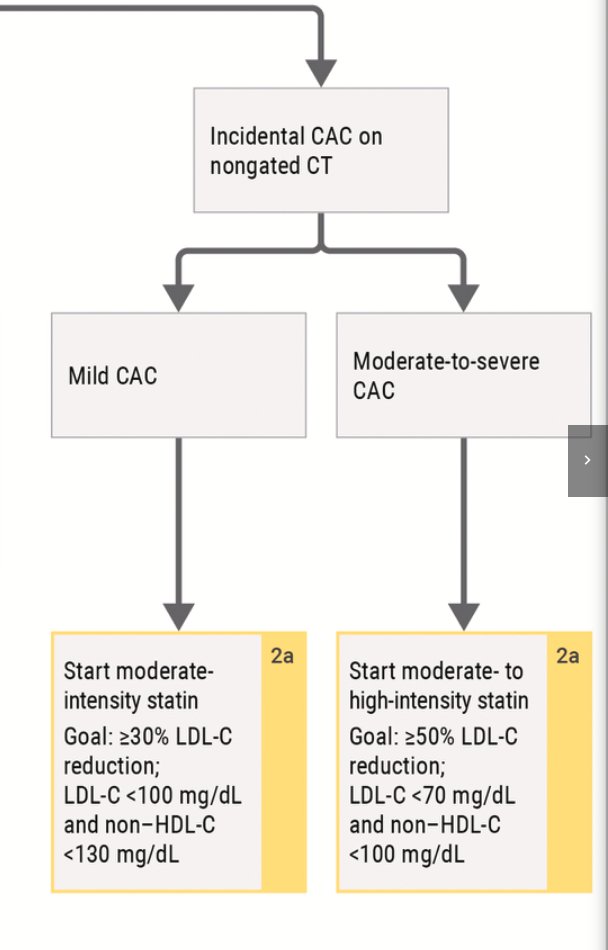


















The software used for this project was Coreline (@CorelineSoft), which also provides AI chest interpretation and adds AI chest findings to calcium scoring in one applications. Recommended by @CotsCardiology. #AI #Cardiology #CalciumScore #ChestCT #MedicalImaging #artificiallntelligence

Regarding the VA AI calcium score study (ai.nejm.org/doi/full/10.10…): Our team at @CVRF_SoCal led one of the first FDA-cleared validation of AI coronary calcium scoring but not from chest CTs (pubmed.ncbi.nlm.nih.gov/37139562/). In 100 non-contrast CACs, AI matched 3 expert readers with R=0.996. Using CAC-DRS calcification system, AI showed 86% agreement; 14% were reclassified—mostly due to underestimating RCA calcium or overestimating RV density for CAC 0–1 which can be clinically relevant to treatment. Overall accuracy of our study: 89%, aligning with the VA study of 84% using chest CT - encouraging for wide-spread adoption. @khurramn1 @CotsCardiology #calciumscore @Heart_SCCT @DrMarthaGulati @EricTopol @RonBlankstein @CVMGBevHills @CAIALOfficial @BudoffMd #artificalintelligence @elonmusk @WHO @BhavikPatelMD @ACCinTouch

AI-CAC enables coronary calcium scoring from routine chest CTs 20K scans, 98 VA sites, 89% accuracy From my perspective, time to connect AI outputs to action, to truly maximize implementation-->prevention ai.nejm.org/doi/full/10.10… #DigitalHealth @HoustonMethodist @RiceUniversity



The revolution in medical science and technology is one of the greatest opportunities for humanity and we’re putting the NHS at the forefront of it. We’ll not only be able to diagnose and treat illness more effectively, we’ll be able to predict and prevent it.


But get this right & it could be transformational for preventative & personalised healthcare. I know – as a father of a child with a rare disease & now through my work at @OHRareDisease – what this could mean. Well done @wesstreeting, keep going!