
Martín Hurtado Felipe
156 posts

@_JMartinHF
Cardiólogo 🇵🇪. Cuidados Intensivos CV 💙 Hipertensión pulmonar🫁. Amante de la ciencia 🧬, música 🎹, cine 🎥.





ICU - Board Review Qs: 60 yo pt admitted to the ICU because of inferior STEMI. Emergency cath: 100% proximal RCA occlusion treated successfully with stenting One hour post-PCI: dyspnea/anxiety - BP: 94/70, HR: 60/min (sinus). Phys exam: JVD (+), clear lungs, cool extremities




El Perú se hizo presente este fin de semana en Burdeos, Francia, en la Olimpiada Europea de Matemática para Mujeres 2026 junto a 65 países de todo el mundo 🇵🇪 Estamos seguros que Dhámaris, Faviana, Gianella y Joyce lo dieron todo en la competencia y en breve tendremos resultados!





Pulmonary artery catheter monitoring in cardiogenic shock a systematic review and meta-analysis #ACVC26 #ACVC_ESC @ACVCPresident @Jorgeheartshock


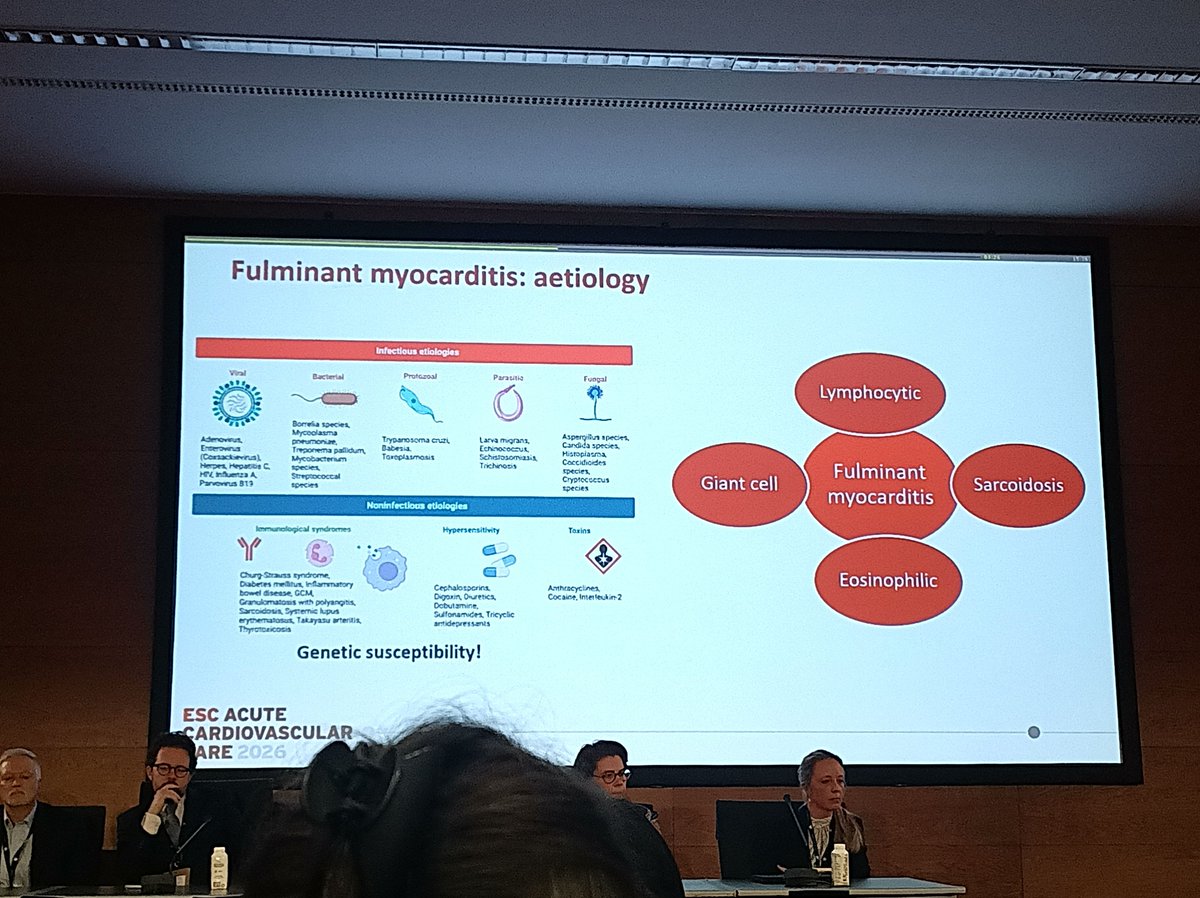

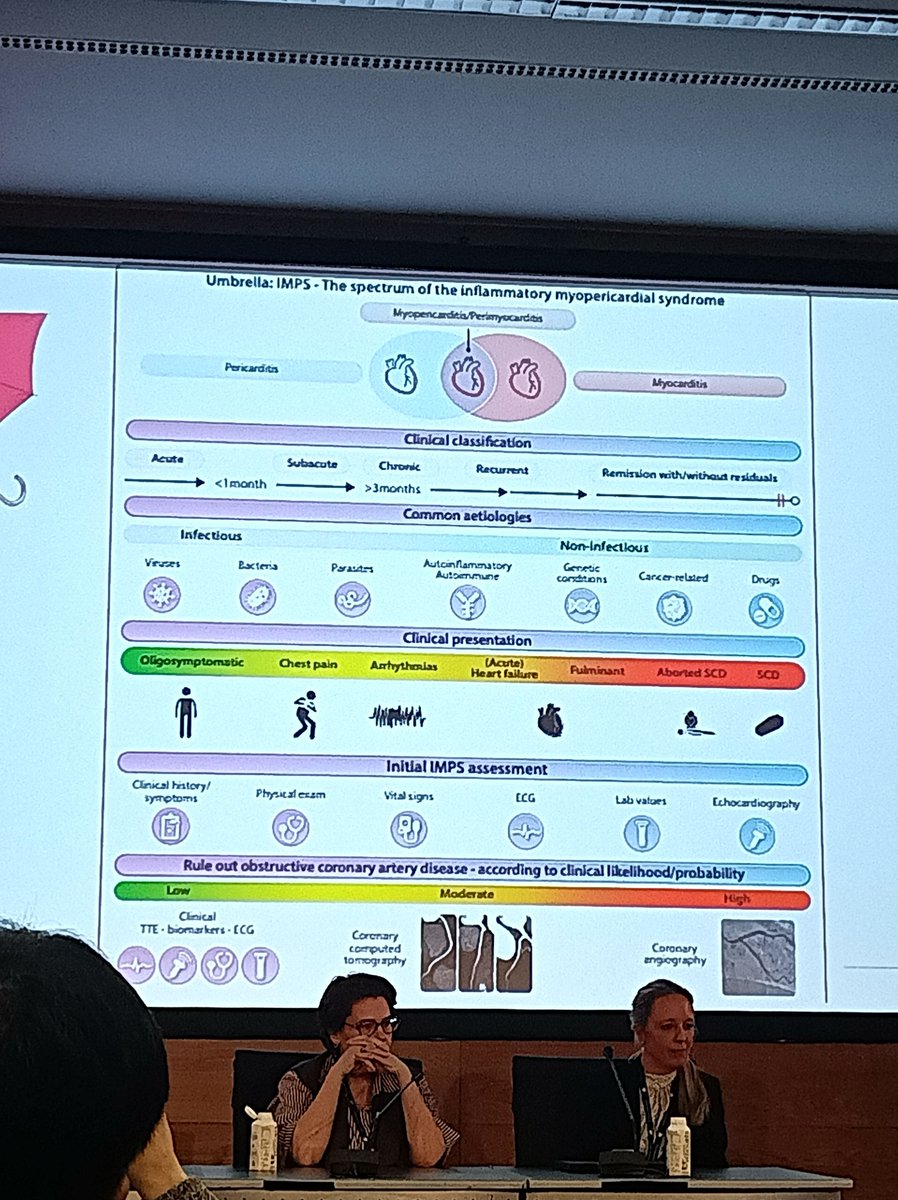



🔴El candidato presidencial Carlos Espá defendió su propuesta de eliminar la Sunedu y planteó que la acreditación sea voluntaria por parte de universidades e institutos. “Creemos en la inteligencia de los estudiantes y sus familias. Cuando un estudiante va a una universidad bamba, lo sabe perfectamente”, afirmó.


El debate en el Congreso sobre la ley de #CuidadosPaliativos mostró cómo una bancada puede distorsionar una política de humanidad: un dictamen para aliviar el dolor y acompañar a pacientes terminales fue convertido por Renovación Popular en una falsa alerta de eutanasia. 🧵


